INTRODUCTION
Heart failure is a condition in which the heart cannot pump sufficient blood and oxygen to supply other organs. It occurs when the heart function is abnormal 1. Heart failure is the leading cause of disease burden and cardiovascular death in many countries worldwide 2. The number of patients with heart failure all over the world is approximately 23 million 3. In Vietnam, an estimation showed that the number of patients with heart failure may range from 320.000 to 1.6 million people according to the global incidence of this disease 4.
Poor treatment adherence in patients with heart failure contributed to the increase in mortality, readmission, and healthcare costs 5. Patients’ adherence to treatment is an important factor for achieving treatment effectiveness. However, many studies have shown that the adherence rate of patients with heart failure remains low. In a study conducted by Monica et al. in 2019, poor medication adherence among Brazilians was 59.9% 6. In Ethiopia (2021), 47.3% of patients did not follow a low-sodium diet, and 52.7% of patients did not limit excess fluid intake 7. In Vietnam, some studies reported slightly low treatment adherence in heart failure patients 8, 9. The research conducted by Sen HTN et al. in 2019 at the Cardiology Department, C Hospital showed that 45.5% of participants had poor adherence to treatment, including non-medication treatment at nearly 20%, and the rates of nonadherence to exercise, limiting excess fluid intake, and daily weight were 56.2%, 66.2%, and 93.9%, respectively 8.
Heart failure also has many impacts on patients’ lives, including fatigue, reduced sleep quality, depression, and reduced ability to participate in normal social activities. These are potential causes of negative changes in the daily lives of patients with heart failure. Heart failure can reduce the quality of life and lead to increased healthcare costs 10. It also has a negative impact on health-related quality of life 11. Hossein’s Pender health promotion model showed that it has an impact on the quality of life among patients with heart failure (p<0.05) 12
Treatment adherence can prevent or delay the progression of heart failure, preventing the occurrence of acute heart failure requiring hospitalization. Therefore, it is important to reduce the number of hospital admissions, alleviate hospital overload, improve patients’’ quality of life, prolong life expectancy, and reduce the economic burden on families and society. However, adherence to heart failure treatment poses a major challenge for patients, their family members, and medical staff. Based on the above facts, we conducted this study to describe the current status of patients’ knowledge, treatment adherence, and quality of life regarding heart failure at Nhan Dan Gia Dinh Hospital.
2. METHODS
The cross-sectional study was conducted from November 2021 to March 2022 at Nhan Dan Gia Dinh Hospital which is a level 1 general hospital in Ho Chi Minh City, Vietnam. The study is the pre-intervention assessment phase of an RCT on patients with HF.
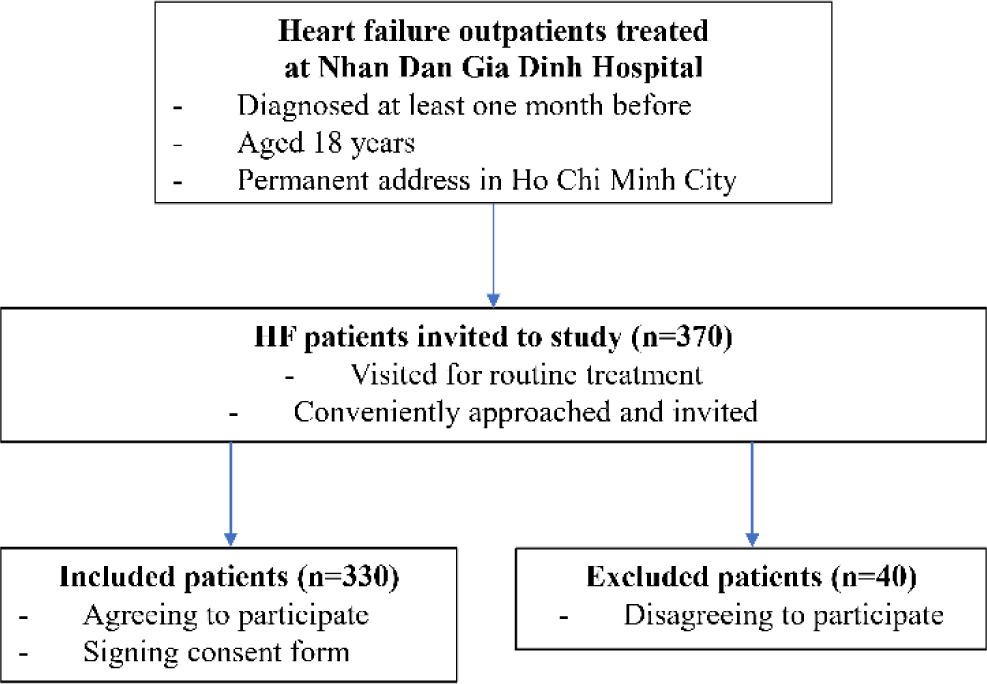
Participants in the study are HF outpatients identified based on an electronic medical record system. In this hospital, heart failure is generally diagnosed based on guide of Vietnam Ministry of Health (no 1857/QB-BYT signed on July 05, 2022). Based on electronic medical records, patients diagnosed at least one month before who were aged 18 years and had a permanent address in Ho Chi Minh City were included in the expected list. On the day before treatment schedules, we called to remind each patient to go to routine treatment. When patients visited for treatment, they were conveniently approached and invited to participate in to study. After finishing the routine treatment, patients were conveniently approached, provided the information about the study, and invited to participate. Patients disagreeing with participating in at least one of the RCT phases (preintervention assessment, implementation of health education intervention, and post-intervention survey) were excluded. Patients agreed to participate by signing the consent form and then were interviewed. Patients who disagreed to participate or had difficulty in understanding or responding were excluded.
Treatment adherence is the main outcome of the study. Therefore, the sample size was estimated to describe treatment adherence prevalence.
In this formula, α is the type I error (α=0.05); Z(1-α/2) is the Z-score of normal distribution at 1-α/2, Z(1-α/2) = 1.96); d is the precision of estimation (d=0.05); and p is the expected treatment adherence prevalence reference from a previous study among HF patients in Ho Chi Minh City Heart Institute (p=32%) 9. The minimum sample size required for the estimation is 335 patients.
The data was collected in the hospital by 20 study staffs who are health care professional. The interviews were based on face-to-face management using a structured questionnaire. All study staff underwent training for patient recruitment, inviting and convincing patients to consent, and interviewing. Before starting the major study, the pilot study on 30 patients was conducted. The pilot result showed the appropriateness of the study protocol, the face validity of the questionnaire, and the interview skills of the study staff.
The study used a structured questionnaire consisting of four parts including general characteristics, HF knowledge, treatment adherence, and quality of life.
General characteristics consisting of the social-economic characteristic and the health condition include age, gender, ethnicity, education level, condition of using health insurance, living with relatives, time from the first diagnosis to study, time from the first diagnosis to treatment, number of emergency hospitalization, HF classification, overweight/obesity (BMI≥25kg/m2), and comorbidities from electronic medical records.
The HF knowledge part is The Dutch Heart Failure Knowledge Scale (DHFKS) consisting of 15 three-choice questions (items) divided into three domains including HF in general (4 items), treatment (6 items), and symptom/symptom recognition (5 items) 13. A patient is given 1 point for each correct answer and 0 point for each wrong answer or missing and the overall score ranges from 0 to 15. We defined adequate knowledge of heart failure (HF) as correctly answering at least two-thirds of the questions in each domain. This means answering 10 or more questions right for the overall scale, 3 or more for the ‘HF in general’ domain, 4 or more for ‘HF treatment’, and 4 or more for ‘HF symptom/symptom recognition’. In a previous study, the DHFKS underwent a back-translation method and was adapted for the Vietnamese context. The Vietnamese version is acceptable reliability with Cronbach’s alpha of 0.72.14
The HF treatment adherence part is the Revised Heart Failure Compliance Scale (RHFCS) consisted of 5 questions (items) about taking medication as prescribed, reducing sodium intake, restricting fluid intake, exercising, daily weighing, and follow-up appointment keeping. Each item was scored by a 5-point Likert scale ranging from 0 to 4 respective never to always compliance (0 = never; 1 = seldom; 2 = half of the time; 3 = mostly; 4 = always). In each item, if a score was either 3 or 4 (indicating a response of ‘mostly’ or ‘always’), we considered that item as adherence. We defined overall adherence as complying with 4 or more items.15 In the Vietnam context, the scale shows Cronbach’s alpha was 0.77 and moderately correlated to HF patients’ mental health (r=0.29).8
HF patient’s quality of life was assessed by EQ-5D-5L v2.1. The scale developed by EuroQol Research Foundation consisted of a descriptive system and a visual analogue scale (VAS). The descriptive system includes five dimensions of mobility, self-care, usual activities, pain/discomfort, and anxiety/depression. This part provides a descriptive profile that can be used to generate a health state value set and identify the health state index (utility score). Health state index generally ranged from less than 0 to 1, with higher scores indicating higher health utility (<0 is worse than dead, 0 is equivalent to death, and 1 is full health). The visual analogue scale (VAS) measures perceived health ranging from 0 to 100 (the worst to the best imaginable health). The advantages of the EQ-5D-5L are cognitively undemanding, taking only a few minutes to complete, and instructions are included in the questionnaire. A study in Germany showed that EQ-5D-5L is a suitable method for assessing health-related quality of life in heart failure patients. The EQ-5D-5L was adapted and developed a value set for the Vietnam population ranging from -0,5115 to 1.16 A previous study in Vietnam used EQ-5D-5L to assess the quality of life in heart failure patients.17
Data were analyzed on STATA v16. We used frequency and percentage to describe almost general characteristics (exclude age, which was analyzed using median and interquartile range (IQR)), HF knowledge, and treatment adherence. Quality of life according to EQ-5D-5L was described by the mean and standard deviation. According to the user guide, EQ-5D-5L can be described by mean ± standard deviation regardless of the distribution assumption.18 The association of social-economic characteristics and health condition with HF knowledge and treatment adherence were tested by Fisher’s exact test and with quality of life by ANOVA test (according to the user guide).18
3. RESULTS
From November 2021 to March 2022, our study approached and invited 370 HF patients. In this, 40 patients disagreed to participate and were excluded. Three hundred and thirty patients agreed to participate and were included in the analysis. The response rate was 89.8%.
The results showed that almost (higher than 95%) patients were Kinh, living with relatives and using health insurance. The gender balance between males and females with a gender ratio approximate of 1:1 (50.3% male and 49.7% female). Elderly patients contributed to the most study sample. More than 60% of patients were aged 60 years or higher. The patients were at a high education level consisting of 48.8% finishing high school and 16.1% finishing at a level higher than high school. (Table 1)
Almost patients were at a low NYHA classification of heart failure. About 57.3% were class I, 24.5% were class II, and only 18.2% were more severe than class II. They were diagnosed less than five years ago, and 45.3% were around two years. About 89.7% of patients were treated in the diagnosed year. Comorbidities were common among the patient, with 91.8% having at least one disease. Hypertension was the most common (73.9%), and the next was dyslipidemia (50%) and diabetes (23.6%). (Table 1)
The study showed the limit of heart failure knowledge among patients. The mean knowledge score of heart failure was 5.2 ± 2.3. Only 4.8% of patients were adequate overall heart failure knowledge. For three dimensions, general heart failure knowledge was best, however, only adequate in 21.8% of patients. The knowledge of HF treatment and symptoms/symptom recognition was lacking; less than 10% of patients had adequate knowledge. Some poorest knowledge recognized by items having less than 20% of patients made correct answers were included “What can cause a rapid worsening of heart failure symptoms” (8.8%), “What is the best thing to do when you are thirsty” (8.8%), “Why should someone with heart failure follow a low salt diet” (13.6%), “How often should patients with severe heart failure weigh themselves” (18.8%). (Table 2)
The study found an association between age and education level with HF knowledge. Knowledge of patients less than 50 years old had better than others (p<0.001). A higher education level was related to a higher HF knowledge (p=0.012). (Table 5)
Overall adherence was only reached by 20.9% of patients. “The compliance on taking medication as prescribed” and “follow-up appointment keeping” achieved highly compliant (93% and 69.4%, respectively). Behavioral compliance was at a low level with only less than 50% patient compliant for each item. Only 12.7% of patients were compliant with restricted fluid intake and 22.4% were compliant with daily weighing. (Table 3)
Only NYHA HF classification was associated with HF adherence. The compliance rate of NYHA class I is higher than others (p=0.016). (Table 5)
The patient’s quality of life was generally stable at a high level, with the EQ-5D-5L reaching a high score. The means of descriptive system score were 0.871 on the scale ranging from -0.5115 to 1, and of VAS score was 69.7 on a scale ranging from 0 to 1, corresponding to and VAS. (Table 4)
| Quality of life according to EQ-5D-5L | Mean ± SD |
|---|---|
| Descriptive system overall score (utility score) (ranging from -0.5115 to 1) | 0.871 ± 0.227 |
| VAS score (ranging from 0 to 100) | 69.7 ± 12.2 |
The study did not find the factors associated with the descriptive system score. For the VAS score, higher age was associated with a higher VAS score (p=0.001), and less emergency hospitalization was associated with a higher VAS score (p<0.001). (Table 5)
4. DISCUSSION
Patients in our study represented many conditions of Heart failure patients as aged and comorbidity. More than 60% of patients were aged 60 years or higher. Almost patients had at least one comorbidity (89.7%). Frequent comorbidities included hypertension was the most common (73.9%), and the next was dyslipidemia (50%) and diabetes (23.6%). These results were similar to many previous studies. Comorbidity prevalence found in the study of Nguyen BT19 was 100%, and in the study of Zeng W20 was 89.8%. Hypertension was the most common in HF patients in these studies with 78% in the study of Nguyen BT19 and 73.9% in the study of Zeng W20.
Almost patients in our study were at low NYHA classification, were diagnosed less than five years ago and 45.3% were diagnosed around two years. They were treated in the first year of diagnosis. The health condition of HF patients was stable, while only 15.8% were emergency hospitalized twice or more around the previous year. Our patients showed milder heart failure than patients in previous studies. NYHA class III accounted for 65% of patients according to Nguyen BT et.al19 in 2016, 73.6% according to Le HN et.al.21 in 2018, and 47.2% according to Dao TP et.al.22 in 2021. Our results revealed the good capacity for HF diagnosis and management at Nhan Dan Gia Dinh Hospital. Emergency hospitalization was associated with the patient’s quality of life. Emergency hospitalization troubles patients and might lead to a low perception of quality of life. Opposite, a bad health condition may lead to emergency hospitalization and a low quality of life. These relationships were found in the previous study with an independent association between quality of life and readmission among heart failure patients.23,24 The diagnosis and management advantage of Nhan Dan Gia Dinh Hospital should be promoted for the patient’s health and quality of life.
Our study showed the limit of knowledge among HF patients. The mean overall heart failure knowledge score (DHFKS score) was 5.2 ± 2.3. Only 4.8% of patients were adequate heart failure knowledge. This result was lower than that in previous studies in Vietnam. The mean DHFKS of Vietnamese heart failure patients was 9.2 ± 3.1 according to Hanh NH25; 7.7 ± 3 according to Binh CT26; 8.7 ± 2 according to Ha TT27; and 8.6 ± 2.1 according to Dinh HTT28. The adequate overall HF knowledge in our study was 4.8%, lower than 17.2% in the study of Xoan VT29 and 27.3% in Ha TT27 Heart failure knowledge in our study was lower than in previous studies in Vietnam might cause some difference in social-economic characteristics and health conditions.
Patients in the studies of Dinh HTT28 and Xoan VT29 were severer HF, younger, and were diagnosed near than our study. According to Dinh HTT28, there were 65% at NYHA class III or IV, mean age of 54.4 years old, 46.4% were diagnosed around one year, and 22.1% were diagnosed around three months before. According to Xoan VT29, 57% of patients at NYHA class II or higher, 51.7% older than 60, and 30% were diagnosed around one year before. Patients having severe conditions or nearer diagnosis might be more impressive to heart failure knowledge than others. Older age might be a barrier to HF knowledge among patients. In our study, education level was associated with HF knowledge with an improvement of HF knowledge by education level (p=0.012). Our study found 64.9% of patients were from high school, that in studies of Dinh HTT28 and Xoan VT29 were about 70%. Although our patients had higher education levels than other studies, HF knowledge in our study was lower. HF knowledge is medical knowledge, different and more difficult to master than lived knowledge. The education level is fundamental to health literacy, and health education is needed to promote knowledge in HF patients. In our study, some poorest knowledge should be concerned in health education programs for patients with HF. These items included “What can cause a rapid worsening of heart failure symptoms” (8.8%), “What is the best thing to do when you are thirsty” (8.8%), “Why should someone with heart failure follow a low salt diet” (13.6%), “How often should patients with severe heart failure weigh themselves” (18.8%).
In our study, the treatment adherence rate of heart failure patients was 20.9%. This was lower than 37% in studies of Nhan LH21 and 54.5% in Sen HTN8. In addition, adherence to medical treatment was high at 75.6%. This was similar to the study of Sen HTN8 in 2019 at the Department of Cardiology, Hospital C, with more than 80% of patients adhering to medication treatment. This is higher than that reported by Monica et.al.6 conducted in 2019 in Brazil showed a drug adherence rate of 41.1%. Good adherence to medication helps doctors control the symptoms of heart failure and prevent worsening. In this study, the compliance rate with limiting fluid intake was 12.7%, which was slightly low. Compared to a study conducted by Nieuwenhuis et al., the rate of fluid restriction intake was 72%-89% during 18 months of follow-up30, which was also reported by Mantovani VN et al. at 40.6% 31, and Phuong DT et al. was 48.4% in 202122. The rate of adherence to a low-salt diet in this study was 42.4%, which is similar to that reported by Nieuwenhuis et al. in 2012 (50%) 30. Research conducted by Ha Thi Thuy in 2021 showed that 32.2% of patients did not or very little follow a salt-reduced diet, and 65.7% of patients did not order low-salt foods when eating out 27. In addition, the patient’s exercise compliance rate was 33.6%, and the daily weight monitoring compliance rate was 22.4%, which is higher than the results of Tam NB19, where only 3.7% of patients always monitored their weight daily and 2.4% of patients adhered to exercise treatment. Adherence to non-drug treatment is more complicated than adherence to drug treatment, which may be the main reason for the low adherence to non-drug therapy.
The study results indicate that treatment adherence in heart failure patients was limited, and non-drug compliance is still more complicated than medication adherence, which has also been found in previous studies19, 22, 32, 30 This study illustrates the necessary strategies to support and strengthen health education regarding HF treatment adherence in patients. Additional to the limitation of adherence in almost patients, our study found that a severer NYHA class was associated with less adherence (p=0.016). Therefore, all patients should be centered in support programs, especially patients with NYHA class III. In terms of support programs, calling or sending letters to remind participants to check and take their medications regularly can improve adherence rates. In addition to increasing knowledge about heart failure, drug, and non-drug treatments can improve patients’ health and quality of life. In addition, having sufficient knowledge helps patients with better self-care and treatment, preventing or slowing the progression of heart failure, and avoiding acute heart failure, thereby reducing the number of hospitalizations and hospital overload, and reducing the economic burden on families and society at the same time.
Quality of life is a factor used to evaluate the effectiveness of treatment in patients with HF. Therefore, this should be considered when monitoring patients undergoing outpatient treatment. Based on EQ-5D-5L, our study recognized the high quality of life on the descriptive system score (0.871 ± 0.32) and VAS score (69.7 ± 12.2). The quality of life scale were measured by five dimentions, including walking, self-care, routine activities, pain/discomfort, and anxiety/melancholy that more affected with the severe HF patients. In our study, most of the patients were low-mild severe HF conditions (81.8% in NYHA class I or II), therefore, they are likely less affected by the above five dimensions of the quality of life scale.
This study has several limitations. First, The study design is cross-sectional and aims to describe the knowledge of heart failure, treatment adherence, and quality of life of the HF patients. Therefore the current data are not sufficient to prove the causative association between higher knowledge of HF resulted in higher treatment adherence and hence increased the quality of life. It warrants further study to access the causative association between knowledge of HF, treatment adherence, and quality of life. Second, the study focuses on outpatients at a single center, suggesting the findings might not be universally applicable to other patient demographics with different characteristics compared to our study population. Finally, the EQ-5D-5L is not designed specifically for accessing the quality of life of HF patients; hence future study needs to consider developing a more specific quality of life scale for HF patients.
Conclusion
Heart failure (HF) is a chronic disease that affects the daily life of patients and requires long-term treatment. Treatment adherence is a crucial issue in controlling the patient’s health. This study showed that the compliance rate was slightly low, especially for nondrug adherence. Very few patients with heart failure have adequate knowledge of the heart failure condition. More support and health education programs on heart failure treatment adherence are needed for patients to increase their knowledge and improve their quality of life.