1. INTRODUCTION
Epilepsy is a chronic disease affecting humans since ancient times and up to now, it remains as one of the diseases that causes the most severe disabilities. Epilepsy affects patients’ activities as well as their family for a long period of time and impairs significantly their quality of lives [1]. Children with epilepsy are often more affected psychologically and socially than children with asthma although both are chronic diseases [2]. This shows that such problems in children with epilepsy are not merely caused by their living with a chronic medical condition [3]. Current studies on epilepsy in the world in general and in Vietnam in particular mostly still revolves around such classic problems as pathophysiology or treatment effects without paying adequate attention to the patients’ quality of life [4, 5]. Evaluation of epileptic patients’ lives provides important information related to treatment and helps to improve treatment quality [6].
In recent years, clinicians have paid more attention to the health-related quality of life (HrQOL) issue of patients with epilepsy and developed various instruments to assess this factor. There are many studies on how to measure HrQOL in adult and children with epilepsy in the world. Recently, measurements of HrQOL have been accepted to take not only a descriptive role but also instrument to measure the results of studies on the efficacy of treatment and management of epilepsy in patients [7].
Quality of life, in general, is considered a social category, which is ruled by each country’s culture, tradition, and ideology. Therefore, results from the studies of other countries cannot absolutely apply to Vietnam society. In Vietnam today, there is still not a Vietnamese version of measurement of HrQOL in epileptic patients to be utilized locally. Among instruments have been developed and validated to assess the quality of life of children with epilepsy, the Quality-of-life Measure for Children with Epilepsy (CHEQOL-25) of Gabriel M. Ronen et al [8] have many advantages: (1) psychometric properties are fully proven, (2) both version for parent-proxy and self-report are available, (3) special structure with alternative paired options of forced responses that have been developed by Harter for “The Perceived Competence Scale for Children” help this instrument more appropriate, more feasible to administer and show less response bias than the traditional Likert scales [8]. This measurement has been translated and adapted into many languages in countries and territories such as Hong Kong [9, 10], Malaysia [11], etc. Therefore, we decided to translate and cross-culturally adapt this instrument into Vietnamese and assess the reliability of the translated versions.
2. METHODS
We selected epileptic patients in the age ranging from 8 to 15 years old with epilepsy duration greater than 6 months, normal psychomotor development for their age, and without other chronic diseases. Patients and their parents/caregivers had an ability to read and understand Vietnamese, and agree to participate in the research. The study was performed at neurology outpatient clinic of Children Hospital No. 2 - Ho Chi Minh City.
Research approval was obtained from the Ethics Committee of University of Medicine and Pharmacy at Ho Chi Minh City, Vietnam.
The instrument which was used to assess the HrQOL of children with epilepsy in our research was CHEQOL-25 of Ronen et al [12]. One of the advantages of this measurement is the inclusion of both self-report version for the child and parent-proxy version for their parents/caregivers. Each version includes 25 items which are divided into five subscales. The score range for each item is 1-4 and for total score is 25-100. The higher the score of scale, the better HrQOL was children with epilepsy. Subscales of each version were presented in Table 1.
Permission for translation was obtained from McMaster University in November 2016 (via email with a representative). The license of using the instrument was purchased on December 1st, 2016.
The translation and cross-cultural adaptation of the original version of the CHEQOL-25 measurement to Vietnamese were performed according to the Principles of Good Practice for the Translation and Cultural Adaptation of Patient-Reported Outcomes Measures of International Society for Pharmacoeconomics and Outcomes Research (ISPOR), which included preparation, forward translation, reconciliation, back translation, back translation review, harmonization, cognitive debriefing, and finalization [13].
We developed two independent forward translations and all forward translators, one is a member of the study group and the other is English expert without knowledge about medicine, were native speakers of Vietnamese. Reconciliation of these forward translations into a single forward translation resolved discrepancies between the translations and sought agreement between individual speech habits and preferences [13]. From the reconciled translation, two Vietnamese translators developed two independent back translations. The review of the back translations to ensure the conceptual equivalence of the translation involved Prof. Gabriel M. Ronen - the author of the original instrument. The cognitive debriefing was conducted on five children with epilepsy and their parents/caregivers at neurology outpatient clinic of Children Hospital No. 2 - Ho Chi Minh City. Participants were requested to read the questions and evaluated difficulty in explaining the meaning as well as the structure of each item and give feedback about the clarity and appropriateness of all items.
Potential patients were screened and the ones who satisfied the inclusion criteria were recruited. After being explained about study’s objectives, methodology and conditions of participation, the patients’ parents/caregivers would sign the informed consent if they agreed to take part in the research.
Parents/caregivers were instructed to complete a questionnaire including three parts: demographic information, characteristics of epilepsy disease and the patient’s quality of life using parent-proxy CHEQOL-25 measurement. Patients were instructed separately to complete a self-report CHEQOL-25 measurement in another room away from their parents/caregivers. The researcher was always available to ensure all the questions on the questionnaire were understood clearly and completed by the participants.
The patients and their parents/caregivers filled in the questionnaires twice, the first time was on their first visit and the second time was four weeks later. We used the same CHEQOL-25 measurement for both times.
Data entry and statistical analysis were conducted using Microsoft Excel 2013 and SPSS version 23.0.
Internal consistency of each subscale was measured using Cronbach’s a coefficient. In this research, Cronbach’s a > 0.70 was considered adequate internal consistency. However, Cronbach’s a > 0.90 suggests redundancy of items [14]. Items in each subscale were assessed by corrected item-total correlation. Items with corrected item-total correlation from 0-0.19 may indicate that the question is not discriminating well, from 0.2-0.39 indicate good discrimination and greater than 0.4 indicate very good discrimination.?
Test-retest reliability or reproducibility was analyzed by intra-class correlation coefficient with ANOVA test. A p-value < 0.05 was considered as statistically significant. The closer the ICC value is to 1.0, the better the test-retest reliability. ICC values > 0.75 indicate high reliability, from 0.5-0.75 indicate medium reliability, and < 0.5 indicate low reliability [15]. Similar research accepted ICC value higher than 0.7 or 0.6 [8, 10]. In this research, we accepted a subscale with ICC higher than 0.6.
ICC was also used to determine the level of agreement between parent-proxy and self-report version [12, 16]. ICCs < 0.40 indicate poor to fair agreement, 0.41-0.60 as moderate agreement, 0.61-0.80 as good agreement, and 0.81-1.00 as excellent agreement [12].
3. RESULTS AND DISCUSSION
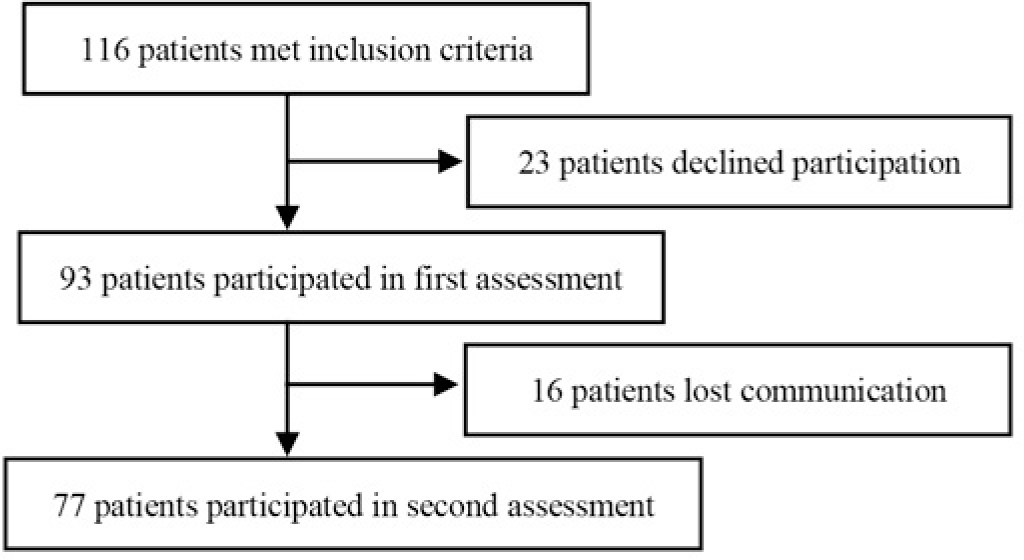
In this research, there were 116 patients satisfied inclusion criteria, 23 patients declined participation and 93 patients agreed to join in first assessment (valid response rate: 80.2%). In the second assessment four weeks later, there was 16 patients lost communication. Therefore, a total of 77 patients administered twice and included in this research. The flow of participants was shown in Figure 1 and the demographic as well as epilepsy characteristics of the sample were shown in Table 2.
In the parent-proxy version, Cronbach’s a for each subscale was greater than 0.7. The subscale with the lowest Cronbach’s a was “Present worries” (0.826) and the one with the highest Cronbach’s a was “Interpersonal/Social” (0.847). All items had a corrected item-total correlation value of > 0.2 (Table 4)
In the self-report version, both the “Present Worries” and “Epilepsy secrecy” subscales had the low Cronbach’s α, 0.651 and 0.681, respectively, whereas, for the other scales, this coefficient exceeded 0.7. All items had a corrected item-total correlation value of > 0.2 (Table 4).
Regarding the test-retest reliability, Table 5 shows that the ICC for each subscale of the parent-proxy and self-report CHEQOL-25 was in the range of 0.77 to 0.98 and 0.61 to 0.86, respectively. The condition of ICC > 0.6 was satisfied for all subscales of each version.
Moreover, with ICC between parent-proxy and selfreport version ranging from 0.35 to 0.62, most of the subscales had an acceptable level of agreement in the rating HrQOL of patients and their parents/caregivers, except for “Intrapersonal /Emotional” subscale (Table 6).
| Subscale | ICC | p |
|---|---|---|
| Interpersonal/Social | 0.62 | < 0.001 |
| Present worries | 0.66 | < 0.001 |
| Intrapersonal/Emotional | 0.35 | 0.001 |
| Epilepsy secrecy | 0.44 | < 0.001 |
In this research, the Vietnamese translation of the CHEQOL-25 was performed according to international guidelines [13]. Backward translation review for Vietnamese versions of CHEQOL-25 measurement was performed by Professor Gabriel M. Ronen of McMaster University, Canada. Cognitive debriefing process conducted on 5 patients to assess comprehensibility, clarity, and appropriateness of each item. The content of each item was familiar with Vietnamese people so no changes necessary. The questions’ structure with Harter’s format was special and uncommon to most research participants. However, after the detailed instruction for the first 2-3 items, the remaining questions were completed without any problem. This indicated our Vietnamese version measurement reaches semantic and content equivalence to the original version.
In this research, Cronbach’s a of each subscale had values > 0.7, which indicate that all subscales had very good internal consistency. The higher Cronbach’s alpha showed the higher correlation between items on the subscale, and hence the internal consistency was also higher. The lowest Cronbach’s a value was in “Present worries” subscale (0.826). The previous translation and cultural adaptation research of the CHEQOL-25 also showed that “Present worries” had a Cronbach’s a value lower than that of remaining subscales: 0.72 in the Chinese version of Yam [9], 0.44 in Serbian version of Stevanovic [16] and 0.67 in the Malay version of Wo [11]. According to Wo et al., the reason lead to this may be because the subscale widely assessed many different worries of the child, such as “think about their epilepsy before doing things” (item 6), “their parents are worried that they will hurt themselves” (item 7), “may not be able to go away to camp or similar places” (item 8), and “worry about getting hurt during a seizure” (item 10). Therefore, the internal consistency of this subscale was not as good as another subscale [11]. The corrected item-total correlation values of all items were > 0.2 which indicate that all of them add sufficiently to the internal consistency.
Regarding the test-retest reliability, our data showed that ICCs of all subscales were satisfied the condition greater than 0.6. The result revealed that the score of a parent-proxy version of Vietnamese CHEQOL-25 was stable in 4-week interval.
We found that the subscales of self-report version did not achieve a good reliability like the parent-proxy one. The “Present worries” and “Epilepsy secrecy” subscale had the Cronbach’s α lower than 0.7 (0.651 and 0.681, respectively). For the other subscales, the Cronbach’s α exceeded 0.7. This was identical with previous research. In the original version of the CHEQOL-25 instrument, the Cronbach’s a of these subscales were 0.71 and 0.63, respectively [8]. In the Serbian version of Stevanovic, the internal consistency coefficients of “Present worries” even achieved value 0.44 [16]. However, the higher value of Cronbach’s a is less important than the choice of specific items because an uncorrelated item may not be covered by the remaining items. Elimination of some questions to elevate the value of Cronbach’s a may lead to lost specific life experiences [16]. In addition, similar to parent-proxy version, the corrected item-total correlation value of most items was> 0.4. The lowest corrected item-total correlation was also greater than 0.2. This indicated that the discrimination of all items in the self-report version was good to very good. Hence, we decided to keep all items in the Vietnamese self-report version like original instruments.
Test-retest reliability analysis revealed that the child self-report version showed good reproducibility with ICCs of all subscales were greater than 0.6. The “Interpersonal/Social”, “Present worries” and “Epilepsy secrecy” subscale were most stable and concrete with highest ICC (0.76, 0.80 and 0.86, respectively). For both the “Intrapersonal/Emotional” and “Quest for normality” subscales, the ICC was lower (0.61 and 0.67, respectively) but still satisfied the condition greater than 0.6 of an acceptable subscale. This result was similar to that of the English version of Ronen et al. with the ICC of these subscales were 0.63 and 0.65, respectively.
Our data showed that there was an acceptable level of agreement between parent-proxy version and the child self-report version with most of ICCs ranging from 0.44 to 0.66, which indicate moderate to good agreement, except for the “Intrapersonal/Emotional” subscale. The “Interpersonal/Social” and “Present worries” subscale had the highest agreement with ICCs value were 0.62 and 0.66, respectively. Meanwhile, the “Intrapersonal/Emotional” and “Epilepsy secrecy” subscales had a higher degree of discrepancy. This difference might be explained by the literature which suggests that emotion are harder observed than physical performance, hence good agreement is usually obtained between parent and child when assess physical aspects of HrQOL [12]. Despite the differences between perspectives of parent and child, the aforementioned result of ICCs indicated that Vietnamese parent form of CHEQOL-25 could be used as proxy measure for HrQOL of children with epilepsy in connection with the child self-report version or when the self-report version could not be administered.
Our research had some limitations. The sample size was small, factor analysis was not conducted to assess construct validity, and no other HrQOL Vietnamese measurement was available to test validity. Therefore, when another Vietnamese measurement of HrQOL for children with epilepsy is available, we need to do this research again with a larger sample size to assess fully validity of Vietnamese versions of CHEQOL-25.
8. CONCLUSION
In summary, we translated and cross-culturally adapted the CHEQOL-25 instrument into Vietnamese with both versions for parent and child scoring. This research reported that our Vietnamese versions were easy to comprehend, feasible to administer, and equivalent to the original version of semantic and content. Both parent-proxy and self-report version had adequate good at internal consistency and test-retest reliability to assess HrQOL in Vietnamese children with epilepsy.