1. INTRODUCTION
Vietnamese women typically experience menopausal symptoms for at least one-third of their lives, given that the average age range for menopause is between 48 to 50 years old, and the average life expectancy of Vietnamese women in 2019 was 79.5 years old[1]. Menopause, a natural part of the aging process, marks the end of ovarian function. It occurs when a woman has not had a period for at least 12 months because her ovaries have stopped releasing estrogen[2]. The reduction in estrogen level leads to symptoms in three main areas: somatic, psychological, and urogenital symptoms. The predominant somatic symptoms are hot flushes, night sweats, discomfort in the chest, sleep problems, and joint–muscle discomfort. Psychological and urogenital symptoms include depression, irritability, anxiety, physical and mental exhaustion, sexual problems, bladder problems, and vagina dryness[3]. Moreover, menopause also increases the risk of cardiovascular disease, osteoporosis, and Alzheimer’s disease. These consequences, coupled with a decline in physical health and societal stigma, impair the ability to work and ultimately reduces the quality of life (QoL) of aging women.
The Menopause Rating Scale is one of the most widely used tools to measure menopausal symptomatology and QoL. Developed by the Epidemiology and Health Research Center in Berlin in 1996, this self-administered scale assesses complaints/symptoms of menopausal women under three subscales, evaluates changes in severity of these symptoms over time, and measures changes in pre and postmenopausal therapy. Although menopausal symptoms vary within individuals, there is currently a lack of tools to quantify the severity of these symptoms in Vietnam[4]. Therefore, this research aimed to address this need by translating the MRS and determining the reliability and validity of the VN-MRS.
2. METHODS
The empirical rule of thumbs recommends at least 5 or 10 participants per observation[5] and a sample size of 200 is considered suitable for factor analysis[6]. To evaluate the scale’s repeatability using the intra-group correlation coefficient (ICC - Intra-Class Correlation), the sample size was calculated following Douglas G. Bonett’s formula [7]. Assuming an expected ICC of 0.86[4], a type 1 error is 0.05 and a confidence interval width of 0.2, 27 out of 200 participants were asked to answer the same questionnaire for the second time two weeks after the first survey [8-12].
A convenience sampling was used in this cross-sectional study. The inclusion criteria were women aged 50-59 years old who have a uterus and 2 ovaries. Participants with any of the following conditions were excluded: hormonal medication use within the last 6 months, participation in the preliminary study, medical conditions affecting menopausal symptoms, psychiatric conditions impairing conversational ability, inability to speak and write Vietnamese, or leaving any questions unanswered in the survey.
The MRS was translated into Vietnamese following the procedure from the Berlin Center for Epidemiology and Health Research[13-15]. Experts critically reviewed the translation to ensure cultural as well as linguistic equivalence.
The scale consists of 11 sections and is divided into three sub-scales: psychological, somatic and urogenital sub-scales. Somatic symptoms encompass flushing, chest discomforts, sleep disorders, joint – muscle problems (sections 1, 2, 3 and 11). Psychological symptoms include depression, irritability, anxiety, physical and mental exhaustion (sections 4, 5, 6 and 7). Urogenital symptoms involve sexual problems, bladder problems and vagina dryness (sections 8, 9 and 10). Responses were classified using a five-point Likert scale, with scores ranging from 0 to 4, where 0 represents no or few complaints, 1 represents minor, 2 is moderate, 3 is severe and 4 is very severe. The MRS score is calculated by summing points from all 11 sections, with the final score ranging from 0 (no symptoms) to 44 (extremely severe).
The 36-Item Short Form Survey (SF-36) is a generic, self-reported survey that measures QoL. SF-36 is divided into 8 sub-scales: physical functioning (10 items), social role functioning (2 items), physical role functioning (4 items), emotional role functioning (3 items), mental health (5 items), vitality (4 items), bodily pain (2 items) and general health perceptions (5 items). The final score ranges from 0 to 100, with higher scores indicating less disability and a better QoL[16].
The scale’s internal consistency was assessed using Cronbach’s alpha coefficients, one of the most widely used test scores for consistency, with value ≥0.7 recognized as an acceptable level[17]. Repeatability (test-retest) was assessed by Intra-class Correlation Coefficient (ICC). We used STATA (version 14) to calculate ICC’s estimates and its 95% confidence intervals based on mean-rating (k = 2), absolute-agreement, two-way mixed-effects models). An ICC greater than 0.9 demonstrates excellent reliability[18].
The scale’s validity was assessed using concurrent validity and construct validity. Concurrent validity measures the correlation between test score (severity of menopausal symptoms score) and relevant criteria (QoL of patients). In this study, concurrent validity was measured using Spearman correlation between the new test (VN-MRS) and an existing test (SF-36) to demonstrate whether changes in the severity of menopausal symptoms correlate with changes in QoL. The construct validity confirmed that the VN-MRS measured the construct of menopausal symptoms, and not measuring respondent’s mood, self-esteem, or other constructs[19, 20].
Confirmatory Factor Analysis (CFA) was used to assess how well the 3-subscale model fit the collected data. Fit indices included: Chi-squared statistic (χ2), Root Mean Square Error of Approximation (RMSEA), Standardized Root Mean squared Residual (SRMR), Tucker-Lewis Index (TLI), Comparative Fit Index (CFI). A p value of χ2 ≥0.5 indicates a good model fit. However, the Chi-square statistic is sensitive to sample size, which may lead to model rejection when the sample size is large or lack of power to discriminate between good and poor fitting models when the sample size is small[21]. Therefore, the following indices were used to assess model fit: RMSEA and SRMR less than 0.08, and TLI and CFI greater than or equal to 0.90[21].
3. RESULTS
The participants’ mean age was 54.1 ± 2.95; 64% of participants were 55 or younger, and all were Kinh (Vietnamese) ethnicity. The majority of participants were non-religious (73%), married (96.5%), and had completed secondary education or higher (78%). The primary occupation of nearly 70% of participants was being a housewife, and almost all participants self-assessed their financial situations as “sufficient to live” (98.5%). Most women were in menopause (50%) or pre-menopause (29%) (Table 1).
The VN-MRS demonstrated a good internal consistency, as evidenced by Cronbach’s alpha, and excellent repeatability (ICC = 0.991, 95% CI: 0.981 – 0.996) as seen Table 2. The consistency coefficients for the scale exceeded 0.81, with scores of 0.81, 0.82 and 0.94 for somatic-vegetative, psychological and urogenital symptoms respectively in Table 3.
| Somatic-vegetative dimension | Psychological dimension | Urogenital dimension | Total MRS score | |
|---|---|---|---|---|
| SF-36 | - 0.86 | - 0.78 | - 0.47 | -0.87 |
| P value* | < 0.001 | < 0.001 | < 0.001 | < 0.001 |
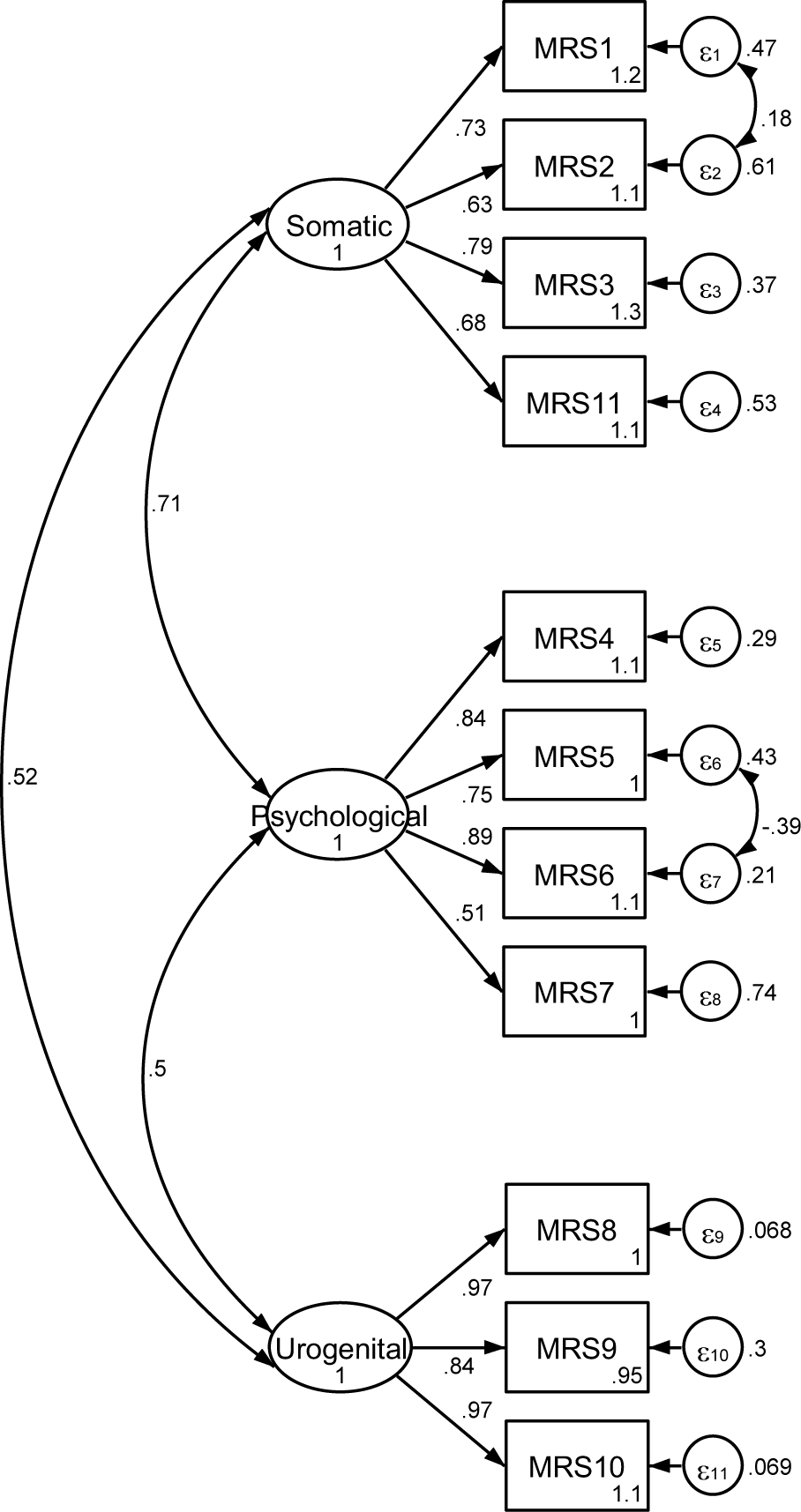
The data from Table 4 suggested that the model aligned with the data collected. The RMSEA ( 0.061 < 0.08, 90% CI: 0.035 – 0.084) in conjunction with other indicators: SRMR = 0.042 < 0.08, TLI = 0.971 > 0.9 and CFI = 0.979 > 0.9, representing a suitable fit. Diagram 1 reveals that standardized factor loading of variables in the VN-MRS ranged from 0.51 to 0.97, indicating that the scale is suitable to use for Vietnamese menopausal women (Figure 1).
| X2 | df | RMSEA (Cl 90%) | SRMR | TLI | CFI | |
|---|---|---|---|---|---|---|
| Original 3- variable model (adjusted) | 67.78 p = 0.003 | 39 | 0.061 (0.035 – 0.084) | 0.042 | 0.971 | 0.979 |
There was a statistically significant correlation between age group and MRS score is (p < 0.001) in Table 5; specifically, people that were 55 or older had higher MRS scores (more severe symptoms) than their peers aged 50 – 55 years. Additionally, a strong inverse correlation was found between education level and MRS score (p < 0.001, r = - 0.68). Moreover, the VN-MRS score reflected stages in menopause, with higher scores correlating with severe stages (p < 0.001 and r = 0.59). This study did not identify any correlation between religion, marital status, socio-economic status and MRS scores.
4. DISCUSSION
The internal consistency results align with those of the original version and other validated versions: Cronbach’s alpha coefficient for the total score in the original version is 0.84, Urdu language version in Pakistan is 0.869[22], Serbian language version is 0.884[23] and the Czech version is 0.87[24]. This indicates good consistency for the VN-MRS and demonstrates cross-cultural applicability of the MRS for assessing menopausal symptoms.
Similar ICC results (ICC ~ 0.9-0.95) were obtained from a study by H. Susanti and colleagues in Indonesia[3].
A strong inverse correlation (r = -0.87, p<0.001) was observed between the QoL measured by SF-36 scale and the severity of menopause symptoms measured by MRS. This suggests that as the severity of symptoms increased, the patients’ QoL worsened. Specifically, concurrent validity coefficients between the SF-36 score and the score of each dimension of MRS ranged from medium to high level (-0.47 to -0.86). Coefficients were higher in vegetative-somatic and psychological scales than urogenital scales, indicating that vegetative-somatic and psychological symptoms have a greater effect on patients’ QoL than urogenital symptoms. Similar results were reported in previous studies, such as research by Tatjana et al (2015) in Serbia[23]. The SF-36 was validated for its reliability and validity in measuring QoL [25].
Standardized factor loadings of this research were similar to the results of the original version in Germany[26]. Correlation coefficient between subscales in the Vietnamese MRS ranged from 0.50 to 0.71, which is consistent with studies from four European countries (coefficient ranged from 0.5-0.6), a North American study (from 0.5 to 0.7), a South American study (from 0.5 to 0.7), and in Asia, especially an Indonesia study that its results ranged from 0.4 to 0.7) [22]. In addition, model’s fitness was also demonstrated through other fit indices: SRMR, CFI, TLI and RMSEA. Thus, we concluded that the Vietnamese MRS exhibits a similar internal structure to the original MRS and is an appropriate tool for measuring the severity of menopausal symptoms.
Women with higher level of education from the study experienced fewer and less severe symptoms during menopause, which is consistent with findings from Jaana M Moilanen and colleagues in Finland on 1165 women aged 45 – 64 [27], and Hoang Thi Lien in Vietnam on 470 women aged 50 - 60 years [28]. This may be attributed to the possibility that women with higher education levels have greater access to healthcare service and more likely to adhere to doctor’s recommendation. Additionally, educated women may be more likely to adopt lifestyle changes, such as diet modifications, based on menopausal symptoms.
In this study, postmenopausal women had higher scores than perimenopausal and premenopausal women. VN-MRS scores increased significantly in correlation to age and menopausal stage, an observation reflected in a study in Ecuador [29] and in Ethiopia [30]. This can be explained by the fluctuating estrogen levels during perimenopause and the decline to deficiency status in the postmenopausal period, causing symptoms to gradually increase. Moreover, menopausal-related changes are negatively impacted by the natural aging process, characterized by a decline in the organ system functions. Therefore, in general, postmenopausal women experience more menopausal symptoms and higher symptom severity.
Previous studies, in Vietnam, have shown associations between factors such as ethnicity, occupation, marriage, economic status and health-related QoL in middle-aged women[31]. However, our study did not reveal an association between menopausal symptoms and these factors. This could be partly due to the homogeneity of our population, as all participants belonged to the Kinh ethnic group, and only a relatively low proportion (only 3.5%) of women were not living with their partners. Menopausal disorder variations are thought to be influenced by regions, living habits and cultures. Therefore, future studies should delve deeper to confirm these associations with menopausal health status.
The research had certain limitations. Firstly, none of the translators in the backward translation process is English native. Secondly, the MRS is a self-reported scale, and the data collection process relies on participants’ memory recall, which can lead to self-report bias and recall bias. In addition, hot weather in the South of Vietnam can influence the accurate assessment of vasomotor disorder symptoms in menopausal women.
Conclusion
This study aimed to validate the validity and reliability of the Vietnamese MRS to assist Vietnamese physicians in classifying the severity of menopausal symptoms. The Vietnamese MRS demonstrates good reliability (assessed by Cronbach’s alpha and ICC) and validity (assessed by concurrent and construct validity), proving its utility as a useful tool for Vietnamese healthcare professionals to make appropriate interventions. Ultimately, the scale’s usefulness lies in its adoption by healthcare professionals and patients. However, it is a common occurrence for aging women in Vietnam to silently suffer from menopausal symptoms. Further studies should be conducted to assess patients’ perception on menopausal symptoms.