1. INTRODUCTION
Carpal Tunnel Syndrome (CTS) is the most common median neuropathy, accounting for 90% of all neurological diseases with a prevalence of about 3.8% in the population [1]. Although CTS is not life-threatening, it has a significant impact on quality of life and medical costs, and there is presently no truly optimal treatment method available. The majority of therapies involve orally administered corticoid or on-site injections; nevertheless, if internal medicine treatment fails or the patients are in a serious situation, they are suggested for surgical treatment. Internal medicine therapies, especially those involving corticoid, have many adverse effects, particularly those that affect the digestive system, which is a significant drawback of the treatment method [2]. Clinical trials of CTS treatment are thus urgently needed [3]. Traditional medicine therapeutic methods, including pharmacological and non-pharmacological methods, have been widely used in the treatment of CTS around the world. For patients with mild to moderate conditions, systematic assessments have demonstrated that manual acupuncture (MA) is an effective treatment without affecting the digestive system [4,5]. MA is a type of acupuncture that uses metal needles inserted into accupoints to create curing effects. Hence, the main drawback is that MA causes pain when the needle inserts into the skin. The pain can be increased by inserting the lower points containing the median nerves, especially the Da ling point (PC7), one of the most used points in CTS treatment by methods of acupuncture [4]. Therefore, MA may not be used in some patients with fear of needles or fear of pain. Another modern type of acupuncture that can overcome this limitation of MA is laser acupuncture (LA).
LA uses a low-power laser to aim at pressure points instead of needles through the skin to create biological effects and stimulate acupuncture points, according to traditional medicine. Low-power laser has been shown to have a wide range of biological effects in various neurological diseases. Especially for peripheral neuropathy, low-power laser has the effect of enhancing nerve regeneration [6]. The use of LA has been deployed in a variety of pathologies, especially when controlling pains such as headaches and neuropathic pain, as well as various neurological diseases [7]. LA has received approval from the Ministry of Public Health in Vietnam and is frequently used to treat CTS. However, there is a lack of evidence of treatment effects. Hence, our study aims to initially evaluate the LA effect in CTS treatment in terms of pain relief and rehabilitation of finger motor function, as well as the safety of LA.
2. MATERIALS AND METHOD
For four weeks, a before-and-after interventional study, assessor-blinded, was conducted in a group of CTS patients to evaluate the efficacy and safety of LA in the CTS treatment. The study was carried out from December 2021 to June 2022 at Branch No.3, University Medical Center, Ho Chi Minh City.
The study was approved by the Board of Ethics in Biomedical Research at University of Medicine and Pharmacy at Ho Chi Minh City on December 14, 2021, No. 794/HDÐ-ÐHYD, as well as with the informed consent of the participants in signing before participating.
The study was followed the Consolidated Standards of Reporting Trials (CONSORT) and Standards for Reporting Interventions in Clinical Trials of Acupuncture (STRICTA) guidelines for designing and reporting controlled trials [8].
The study included outpatients diagnosed with mild or moderate CTS, in the left or right hand, the diagnosis of CTS was confirmed by electromyography (EMG) [9]. They belong to the age group of 18 years or older, regardless of gender, and do not receive CTS treatment by other methods. Excluding the group of patients with carpal tunnel syndrome in both hands.
The study excluded the following cases: Wrist injury or systemic diseases (rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis, Scheuermann’s disease), as were symptoms of systemic pathology (weight loss, fever with unknown causing, anorexia, personal pathology history of malignant growth, diffuse pain and disseminated ankylosis), symptoms of infection (fever, meningitis, photophobia), symptoms of central motor neuron dysfunction (Hoffmann’s sign, Babinski reflex, hyperreflexia, spasticity, incontinence, genitourinary dysfunction), having contraindication of LA (the affected area is infected, ulcerated, pathology confirmation of cancer) and CTS surgery.
An assessor-blinded study was evaluated by not letting the assessors know whether they were collecting treatment outcome information before or after the intervention. The recruiter will gather fundamental demographic data. Then, one investigator will analyze the disease status data used to assess the treatment outcome prior to the intervention, and another investigator will assess the treatment outcome following the intervention. The placement of participants based on which investigator assessed them before or after the intervention was determined at random and assigned by another investigator (who was also in charge of recruitment).
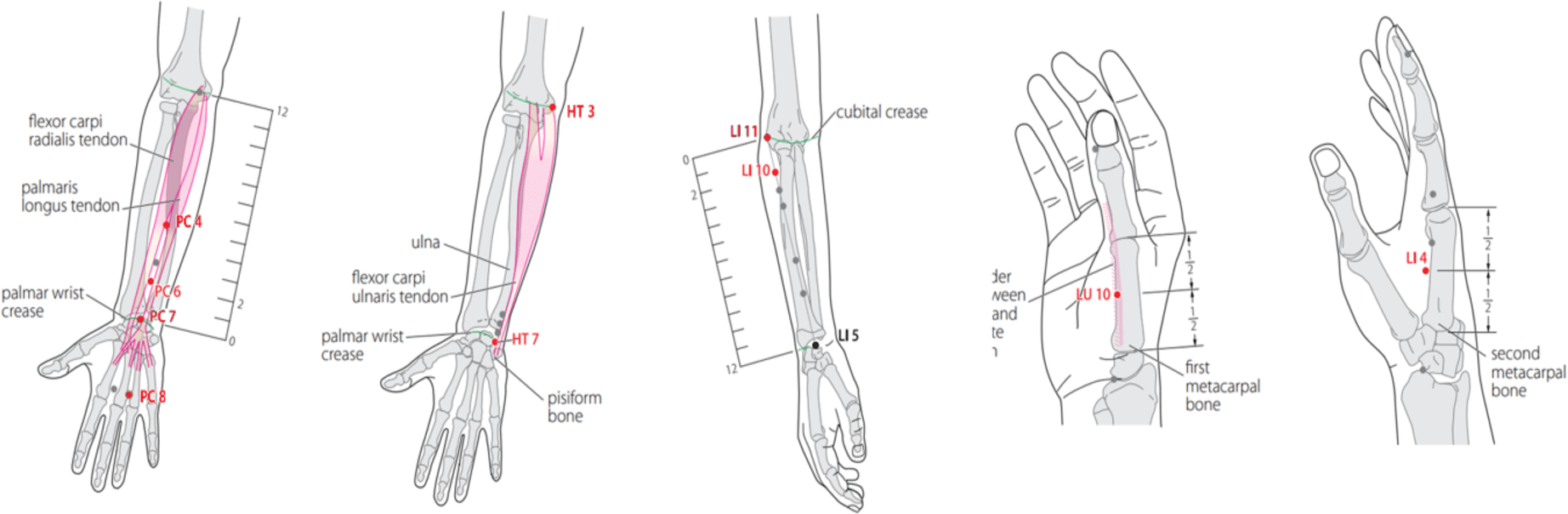
After being selected for the study, the patient will receive an LA treatment for 20 minutes once a day, 5 times a week, continuously for 4 weeks (a total of 20 LAs). The study also included the use of a Lightneedle 600 machine, made in Germany, with a wave-length of 655 nm, continuous wave, wattage of 5 mW for each point (acupuncture point), and a dose of 6 J per point, with the laser beam directed perpendicular to the skin surface. Selected points include PC4 (Xi Men), PC6 (Nei Quan), PC7 (Da ling), PC8 (Lao Gong), LI4 (He Gu), LI10 (Shou San Li), LI11 (Qu Chi), HT3 (Shao Hai), HT7 (Shen Men), and LU10 (Yu Nghi) on the hand side were diagnosed with CTS [10][11]. Point positioning based on WHO standards [12] (Figure 1). All acupoints are treated with LA in the same time. In this study, a doctor with 12 years of experience practicing traditional medicine and 5 years of experience with the LA technique was selected to perform in all cases. The doctor and the patient both wear protective eyewear during the laser acupuncture treatment.
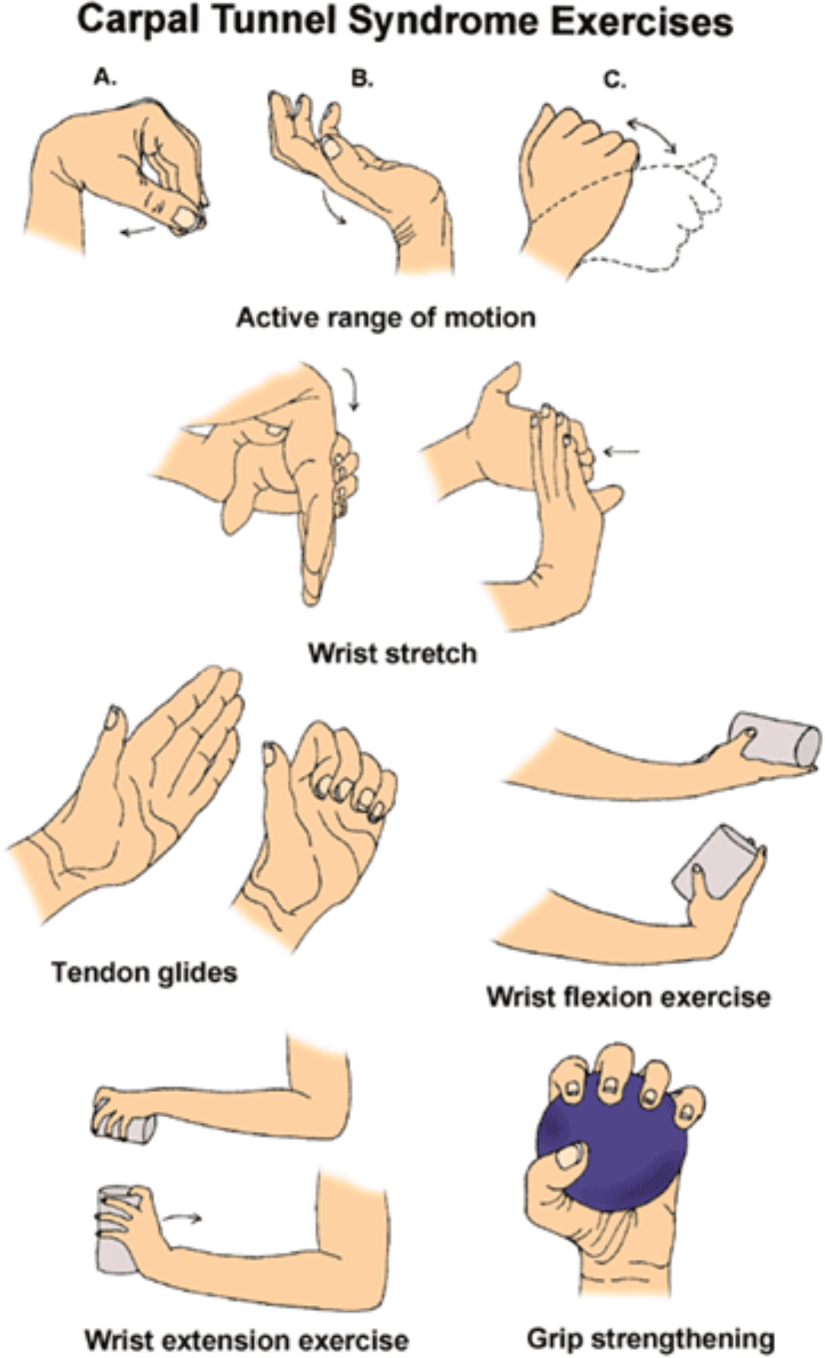
Along with the LA intervention, patients are given instruction on lifestyle changes and wrist-hand exercises simultaneously (Figure 2). This exercise is practiced by the doctor and the patients right after each time the patients are treated with LA.
The change in the Symptom Severity Scale (SSS) and the Functional Status Scale (FSS) when compared to before and after the intervention was the study’s main result. Both of these scores were obtained from the Boston Carpal Tunnel Syndrome Questionnaire (BCTQ). SSS had 11 questions with 5 levels (1–5) corresponding to each level from moderate to the most severe, so SSS is worth 11–55 points. Similarly, the FSS had 8 questions, each with 5 difficulty levels ranging from 1 to 5: no difficulty, little difficulty, moderate difficulty, intense difficulty, and cannot perform the activity at all due to symptoms; the FSS value ranges from 8 to 40 points [13]. The results will be collected from the self-assessment questionnaires, with the help of the researcher’s interpretation when needed. Data will be recorded immediately before the intervention (week 0), after 2 weeks (week 2), and after 4 weeks of treatment (week 4) [10].
Fully symptomatic recovery was determined to be when all 11 SSS questions yielded a score of 1 (moderate), and rehabilitation was determined to be when all 8 conditions in the functional condition of the FSS yielded a score of 1 (no difficulty). The collected data will be recorded after 4 weeks of treatment (week 4).
Adverse events were continuously monitored throughout the intervention, including the following variables: tingling, transient dizziness, headache, fatigue, and needle sickness.
The study will be terminated when the patient does not want to continue participating in the study, is intolerant of the treatment method , has serious side effects, or using other methods to treat CTS during the ongoing research.
The sample size was calculated to detect the difference in the effectiveness of symptom score reduction (SSS) with type 1 and type 2 errors at an acceptable level of α=0.05 and β=0.1, respectively (equivalent to 90% of the sample). Depending on previous research on pain relief based on the low-level laser SSS scale and the sample size calculation formula comparing two paired means (before-after), the study required at least 31 participants [14]. Hence, the study needed 38 individuals in order to account for a 20% sample loss.
All analyses were performed on the intention-to-treat (ITT) population of participants. Missing data were replaced with the mode value of the corresponding group. These cases would be considered as treatment failure. Data analyses were performed with the use of the statistical software STATA 14.0 Primary outcomes were presented as mean with standard deviation (SD) or median with interquartile range (IQR 25th-75th) and were tested for difference between before and after relying on parametric and non-parametric tests depending on the data characteristics. Secondary outcomes were presented as frequencies and percentages (%) and with 95% confidence intervals. The significant level was set as p<0.05.
3. RESULTS
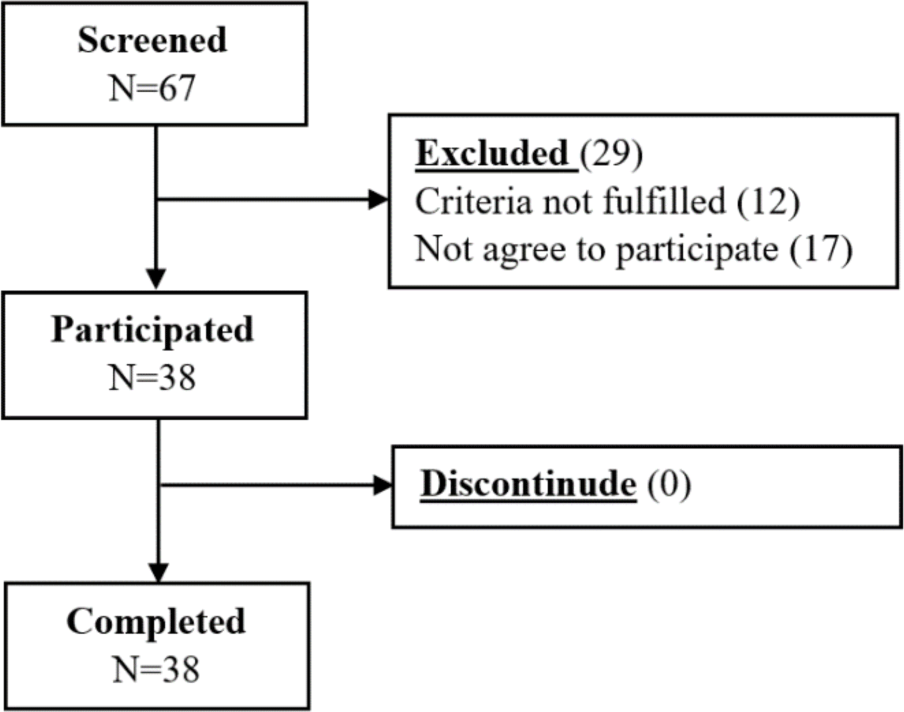
Study recruitment commenced on December, 2021 to June 2022 when the number of subjects reached the recruitment goal. In total, we approached 67 patients, of which 12 patients did not meet the inclusion criteria or met the exclusion criteria, and 17 patients did not agree to participate in the study. In the end, the study recruited 38 patients. During the treatment intervention, there was no patient that lost to follow-up. The sample selection process is shown in Figure 3.
The baseline demographic and clinical characteristics are shown in Table 1.
Occupations requiring more than 20 hours of computer work per week (office worker, accountant, information technology engineer); occupations requiring hand vibration pressure (canning workers, construction workers, shoemakers, tailors); occupations requiring wrist pressure greater than 4 kg; occupations requiring repetitive hand work (driver, doctor, pharmacist, teacher, lecturer) [15,16,17].
Participants, more than two-thirds of whom are women, have an average age of about 43 years, of which the majority are between 40 and 59 years old. Over two-thirds of patients work in occupations with a high risk of CTS. Being overweight and having diabetes, which account for 10% of participants, are additional risk factors. In general, the disease occurred in both the right and left hands, and the extent of the disease was quite similar, with a symptom score of 28 (27–33) and a functional score of 13 (13–15). All participants in the study had previously received treatment.
The change in SSS scores before and after every 2 weeks of intervention for 4 consecutive weeks is shown in Figure 4.
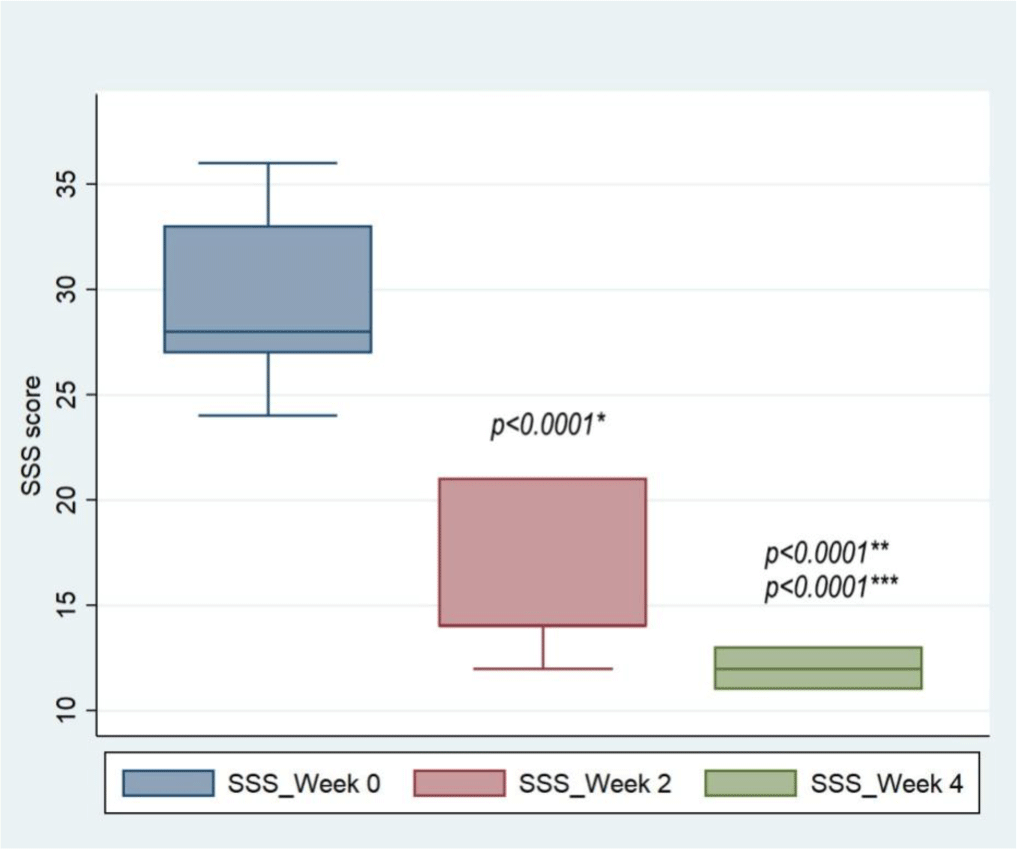
The SSS score was 28 (27–33) before to the treatment intervention, according to analysis results. The SSS score dropped to 14 (14-21) and 12 (11-13), respectively, after 2 and 4 weeks of intervention, and this reduction was statistically significant (p < 0.0001). Comparing SSS score after 2 weeks of intervention with after 4 weeks of intervention, the reduction was statistically significant (p<0.0001).
The change in FSS score before and after every 2 weeks of intervention for 4 consecutive weeks is shown in Figure 5.
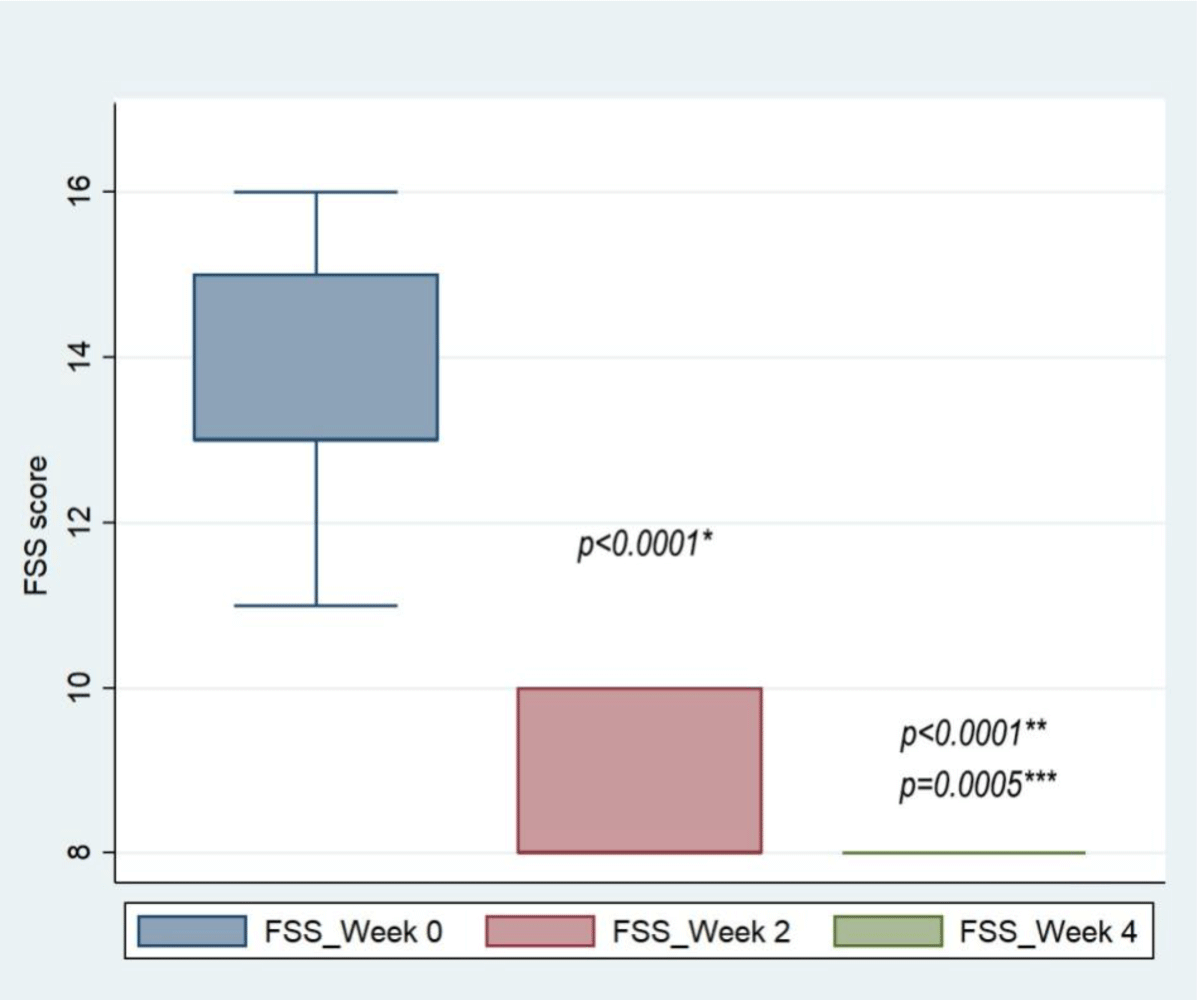
Similar to the improvement in SSS scores, the pre-intervention FSS score was 13 (13-15), dropped to 8 (8-10) after 2 weeks, and then returned to a functionally moderate score of 8 (8-8) after 4 weeks of treatment; the difference was statistically significant (p<0.0001). Comparing SSS score after 2 weeks of intervention with after 4 weeks of intervention, the reduction was statistically significant (p=0.0005).
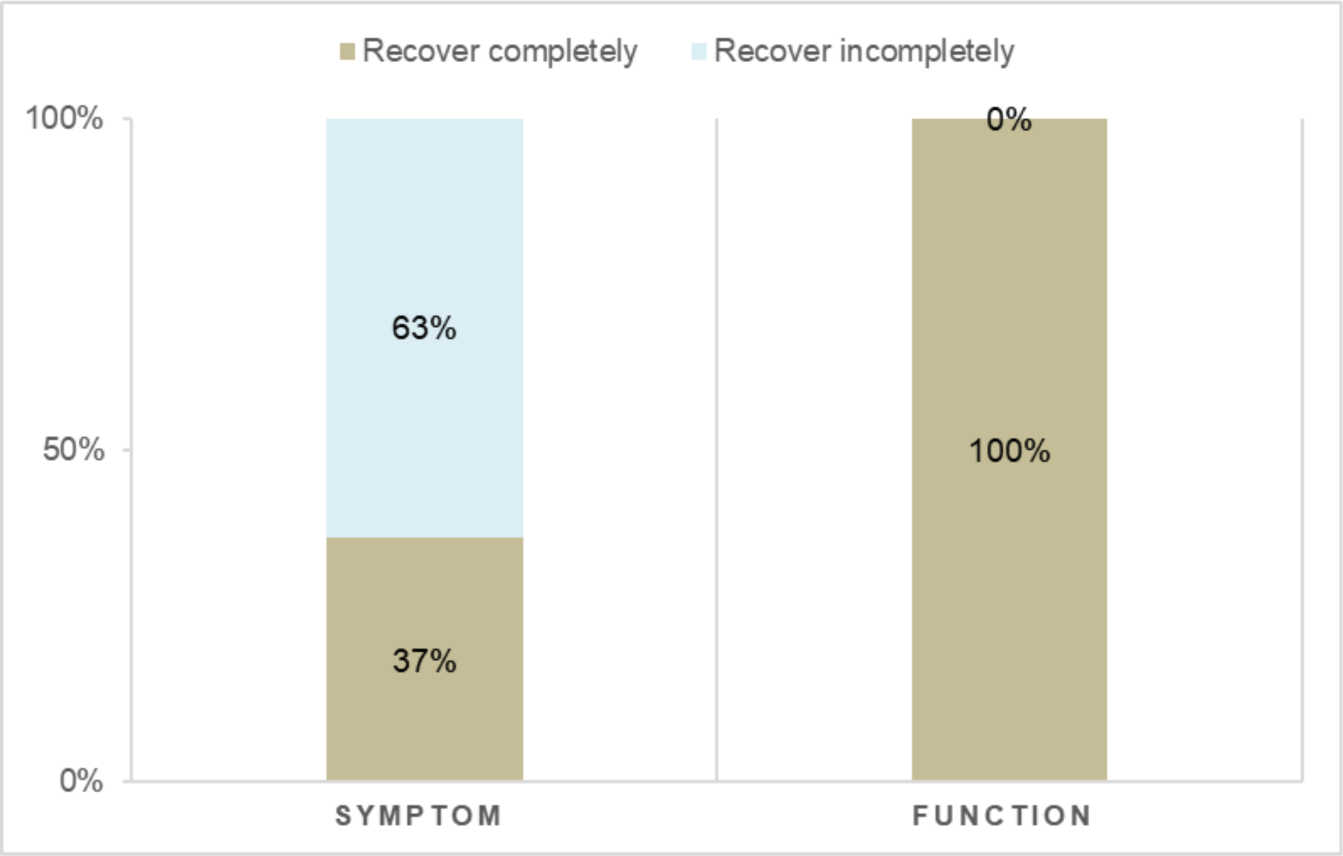
The rate of full symptomatic and functional recovery is shown in Figure 6.
In terms of symptoms, 37% of patients (CI 95%, 23–53%) fully recovered, while 100% of patients fully recovered in terms of function.
4. DISCUSSION
According to our study’s sample characteristics, the percentage of females is much higher than that of males, and the majority of age groups are from 40-59 years old. These features are similar to those in previous reports on the epidemiology of CTS [18]. Most patients had occupations associated with a high risk of CTS, while overweight and diabetes factors also thought to be associated with CTS were present in about 10% of patient [18]. The proportion of mild and moderate conditions was nearly equal, and each question’s mean SSS score was around 2-3, which was quite similar to previous studies of Low-level laser therapy (LLLT) or MA CTS treatments. However, for our research, the FSS scores were 1-2 for each question, lower than in previous studies.
LLLT stimulates biological reactions in a variety of neurological diseases by using low-power laser with wavelengths ranging from 632 to 1064 nm. LLLT has the role of enhancing nerve regeneration, increasing axons containing myelin sheaths, and gradually improving motor function in peripheral neuropathies [6]. Numerous clinical trials on CTS show that LLLT reduces symptoms through improved SSS and improves functional recovery through improved FSS, as well as improving electrophysiology on electromyography (EMG) when used monovalent or in combination with other therapies [19,20,21,22]. However, the mixed results indicate that the evidence from the studies is weak, and no clinical data to support the use of LLLT in the treatment of CTS have been discovered [23].
These inconsistent results seem to spur research on LA therapy. LA also uses a low-power laser similar to LLLT but will be directed at a special place that has therapeutic effects based on traditional medicine theory called acupoints. LA is expected to bring therapeutic effects based on the biological effects of low-power laser and stimulate acupuncture points, thereby creating therapeutic effects according to traditional medicine theory. Until now, studies of LA in the treatment of CTS have been scarce, but efficacy appears to be consistent. According to Branco et al. (1999) [24], LA combined with other methods can provide significant pain relief. Study by Juan et al. (2019) LA improved overall symptoms more than sham - LA in patients with mild to moderate CTS, and a recently reported case series by Limanjaya et al. (2022) [25] showed that LA improved BCTQ scores and decreased VAS scores. The findings of the research mentioned above resemble those of our study. According to the findings of our study, SSS and FSS scores significantly improved after two weeks of treatment (p<0.0001), and after four weeks of treatment, the improvement was even stronger. Particularly, SSS is decreased from 28 to 12 points, while FSS is decreased from 13 to 8 points (unlimited function). The complete symptomatic recovery appeared to be more difficult than the functional side. Meanwhile, 100% of patients recovered functionally after 4 weeks of LA. This trend was not very clear, and we found variation in several trials of LLLT in CTS treatment [14,19,22]. Differences may result from study heterogeneity in intervention parameters such as wavelength, pulse, power, energy, time, location, and baseline patient characteristics, especially since the pre-intervention FSS score in our study was quite low. Furthermore, in this study, we used LA therapy in addition to shining laser beams at acupoints that coincide with the path of the median nerve, including PC4 (Xi Men), PC6 (Nei Quan), PC7 (Da ling), PC8 (Lao Gong), LI4 (He Gu), LI10 (Shou San Li), LI11 (Qu Chi), HT3 (Shao Hai), HT7 (Shen Men), and LU10 (Yu Nghi),with the expectation of creating many different effects based on the theory of traditional medicine. This acupuncture formula selection effect can also result in rapid functional improvement.
Improvements in symptoms and function of LLLT and LA are often associated with improvements in nerve conduction studies based on EMG. However, Juan et al.’s (2019) [26] LA study on the treatment of CTS revealed that, despite improvements in symptoms and function, there was no improvement in neurotransmission. In contrast, Limanjaya et al.’s (2022) [25] series of case reports demonstrated improvements in symptoms, function, and electrophysiology. This inconsistency may be caused by various baseline and intervention parameters as well as various acupressure formulation options. While Juan et al. (2019) [26] only used two acupoints on the median nerve’s path, PC6 (Nei Quan) and PC7 (Da ling), Limanjaya et al. (2022) [25] added five acupoints on the affected side, including LI4 (He Gu) and four EX-UE9 (Ba xie). Our trial tended to choose acupoints similar to Limanjaya’s study; nevertheless, the effect of electrochemical improvement was not examined in our study. As a result, it is unclear whether the improvements in symptoms and function were accompanied by improvements in electrical conduction on the EMG of the median nerve in this study.
LA offers acupressure treatments that are very similar to MA, with the main difference being that LA uses a laser instead of acupuncture needles. There are many reports showing that MA is useful in the treatment of CTS without serious side effects [4]. Research Tezel et al. (2019) [27] performed MA in 5 consecutive weeks at PC7 (Da ling), PC4 (Xi Men), PC6 (Nei Quan), HT7 (Shen Men), LU9 (Tai Yuan), and Ll11 (Qu Chi) and found an improvement in SSS score from 29.8 to 23.4 and FSS score from 26.8 to 20.7. This improvement seems to be lower than in our study; specifically, SSS decreased from 28 to 12 and FSS decreased from 13 to 8. Besides the differences in the acupuncture formula, the baseline characteristics of the sample make it clear that the more efficient LA trend may come from the combination of low-energy laser effects. However, in order to confirm this hypothesis, an RCT study comparing the efficacy of MA and LA in the treatment of CTS must be designed. Additionally, MA can cause pain, bleeding, and damage to structures such as blood vessels and nerves when punctured due to its invasive character. In contrast, LA is a safe, non-invasive procedure. Previous reports of adverse events noted some cases of tingling, transient dizziness, headache, and fatigue after using LA; however, these effects are rare and mild [7,27]. None of the aforementioned adverse effects, including acupuncture needles sickness, were noted in this study.
Conclusion
The findings of our study point to the possibility of treating CTS with LA by symptom improvement, particularly in terms of function. No adverse effects were observed with LA, indicating its safety in the treatment of CTS. LA should be a reasonable option, especially for patients with needle phobia or those with contraindications to MA. However, the structure of the before - after study, without a focus group means that the effect of treatment may be overstated by the effects of accompanying interventions, including lifestyle changes and exercise, as well as the placebo effect. There is a need to promote RCT trials as well as controlled studies between LA and MA in the treatment of CTS.