1. INTRODUCTION
The breaking out of the COVID-19 pandemics created a tremendous burden for the healthcare system due to many patients in the acute-stage and the dramatically rising persistent symptoms in COVID-19 patients [1]. According to Haverall S et al., 80% of hospitalized COVID-19 patients faced prolonged symptoms, and 10% - 35% non - hospitalized patients had to confront these issues [2]. In managing post– COVID-19 syndrome, many publications, and guidelines have been presented, including applying Traditional Chinese medicine (TCM) in accelerating the recovery pace of post-COVID-19 patients. For instance, An.Y.W surveyed 372 recovered COVID-19 patients, and 191 accepted using TCM. The result pointed out the positive alteration of IL-6 and Gamma-glutamyl transferase and the potential of TMC in these patients [3].
In the TCM, due to the severe damage of yin and qi in the acute phase, recovering patients after COVID-19 showed two common syndromes: deficiency of lung–spleen qi syndrome and qi yin deficiency syndrome. As a consequence, numerous TCM studies mainly focused on the interventions for these syndromes and their impacts on the patients. However, we were deficient in the study of the Eight Principles, which was a crucial instrument to understand the TCM characteristics of the post-COVID-19 syndrome. In TCM, the practitioners use the Eight Principles as a comprehensive approach to understanding the general characteristics of the disease, for instance, yin-yang, cold-heat, excess-deficiency, and internal-external. Using this information, they narrow the scope, identify the pathogen, and also determine the appropriate intervention. Therefore, taking the initial step to widen the outlook on the post-COVID-19 syndrome in TCM, we identified the relationship between the post-COVID-19 syndrome and the cold–heat pattern, which is a part of the Eight Principles. Aiming for this objective, firstly, we determined the anthropometric characteristics and cold–heat pattern of the sample, then, identified the relevance between these factors and post-COVID-19 status.
2. MATERIALS AND METHOD
A cross-sectional study was established at the TCM faculty of UMC from January 2022 to April 2022. The survey was taken by 384 patients presented at UMC during the study period (including outpatients, inpatients, and students). The survey was taken using a convenient sampling method following the inclusive and exclusive criteria. The reporting of this study follows the STROBE guideline [4].
Inclusive criteria:
Currently, there are no previous studies on the relationship between cold-heat patterns and post-COVID-19 syndrome. Therefore, we used P=0.5. We used tolerable error (d) as 0.05; and reliability as 95% which means Z was equal to 1.96. Using the formula, we calculated our sample size:
The questionnaire was in Vietnamese, and the content was based on the Cold and heat pattern identification questionnaire developed by Yeo M et al. (2016) [7]. They evaluated the reliability of the questionnaire by using Cronbach’s α. The Cronbach’s α value of 8 cold questions was 0.79 and of 7 heat questions was 0.83, which was considered to be satisfactory.
They also examined the agreement of diagnosis and coefficient of kappa, and the agreement rate of diagnosis was 64.2%, and the coefficient of kappa was 0.51, which can be interpreted as appropriate. Bae et al. (2018) conducted a pilot study to assess the reliability and the agreement of the experts for the Cold and heat questionnaire. Their result illustrated that the agreements were 82.8% (for cold pattern) and 72.9% (for heat pattern). In addition, Cronbach’s alpha coefficient showed 0.754 (for cold pattern) and 0.753 (for heat pattern) [8]. Bae et al (2018) suggested that the cold and heat questionnaire was a reliable and valid instrument for identifying the cold-heat pattern.
Our questionnaire included three parts: General information (6 questions: Name, Address, Age, Gender, Height, Weight), post-COVID-19 status (3 questions: The day when the patients were confirmed positive for COVID-19, Symptoms appeared or prolonged after confirmed negative for COVID-19, the day when symptoms completely disappeared) and Cold and heat pattern (8 Heat questions and 11 Cold questions).
Age was calculated by the difference between the current year and the participant’s birth year. Age-group was a categorical variable, dividing participants into three groups (Age from 18 to 29: Young adult; Age from 30 to 59: Middle age; Age 60 or older: old age). Gender included male and female. Body mass index (BMI) was calculated based on weight and height. BMI was categorized using the IDI & WPRO standard. The respondent’s answers recorded age and gender, weight, and height.
Post-COVID-19 status was a binary variable including two values: Yes and No. The “Yes” answer required two factors: (1) COVID-19 patients had prolonged or new symptoms after receiving their negative COVID-19–19; and (2) The period - from when they received positive test results of COVID-19 to when all persistent symptoms disappeared or to when the survey day - is equal to more than four weeks.
The Cold and heat pattern was a categorical variable, including four values: Heat, Cold, Combination, and Non-cold–heat. This variable was based on the result of Heat scores (HS) and Cold scores (CS). The “HS” was the total score of 7 Heat questions (with the cut-off being 17.5). The “CS” is the total score of 8 Cold questions (with the cut-off being 21.5) [9]. The participants answered each question by scoring from 1 to 5, depending on their own experiences.
| Pattern | Score |
|---|---|
| Cold | HS < 17.5 and CS ≥ 21.5 |
| Heat | HS ≥ 17.5 and CS < 21.5 |
| Combination | HS ≥ 17.5 and CS ≥ 21.5 |
| Non – cold – heat | HS < 17.5 and CS < 21.5 |
At the end of the patient’s appointment, according to the criteria of the study, the medical staff representing the interviewer chose the appropriate individuals to introduce and ask for their permission to conduct the study. For the students’ subjects, the interviewer reached them, presented the study, and asked for their permission directly. The information sheet and purpose of the study were provided and explained to eligible participants. After having the agreement, the interviewer approached them by three methods: face-to-face, by telephone, or by URL link.
Data were analyzed by using SPSS 26. Frequency and percentage were used to describe categorical and binary variables (Gender, Age group, Categorized BMI, post-COVID-19 status, and cold and heat pattern). Median (Q1– Q3) described quantitative variables (Age, BMI) by gender and post-COVID-19 status. If only one or more information in crucial fields of a respondent were missing (Gender, Age, Weight, Height, post-COVID-19 status, and the answers to the 8 cold-questions and 7 heat-questions), the whole data of that respondent would be removed.
Pearson’s Chi-square test was carried out to identify the relationship between Gender or Cold and heat patterns and post-COVID-19 statuses. The T-test or Mann–Whitney U test was used to determine the relationship between Age and BMI with post-COVID-19 status. P–values <0.05 were considered statistically significant.
3. RESULTS
In 4 months, from January to April 2022, we approached 393 patients, and 9 patients did not agree to participate. Consequently, our final samples contained 384 eligible patients who met the inclusive criteria without exclusive criteria. During analysis, 17 samples were considered missing (4.41% of the sample). We detected missing data in 3 fields: randomly blank answers to the 8 cold questions and 7 heat questions (11 samples), the year of birth (2 samples), and the positive and negative-to-COVID-19-result-receive day (4 samples). With the ratio of missing data accounted for less than 5%, the missing data would not affect the final results [10].
| Kolmogorov-Smirnov | Shapiro-Wilk | |||||
|---|---|---|---|---|---|---|
| Statistic | df | Sig. | Statistic | df | Sig. | |
| Age | 0.099 | 367 | 0.000003 | 0.938 | 367 | 0.000000 |
| BMI | 0.075 | 367 | 0.000031 | 0.963 | 367 | 0.000005 |
The median age of the study was 33 (24 - 42), ranging from 18 to 75. Middle age took up 54.5%, while the old age group was the smallest part (4%). About two-thirds of the participants were women (61.31%). More than half of the respondents had normal BMI (56.13%), and the median BMI was 21.97 (19.78-23.88).
In the non-post-COVID-19 group, the proportion of females was 1.1 times higher than males, while the difference between males and females in the post-COVID-19 group was 1.9 times. The P-value was 0.028 (<0.05), which indicated a statistically significant relationship between gender and post-COVID-19 status.
We did the test of normality of Age and BMI. Because the sample size was more than 50, we used the Kolmogorov-Smirnov test. The (Sig.) values of this test was 0.000003 (<0.05) for the age and 0.000031 for the the BMI (<0.05), which means that the age and the BMI did not have a normal distribution. The Age and BMI distributions had no difference between having post-COVID-19 and non-post-COVID-19 groups. Both BMI and age had no relevance to post-COVID-19 status (p>0.05).
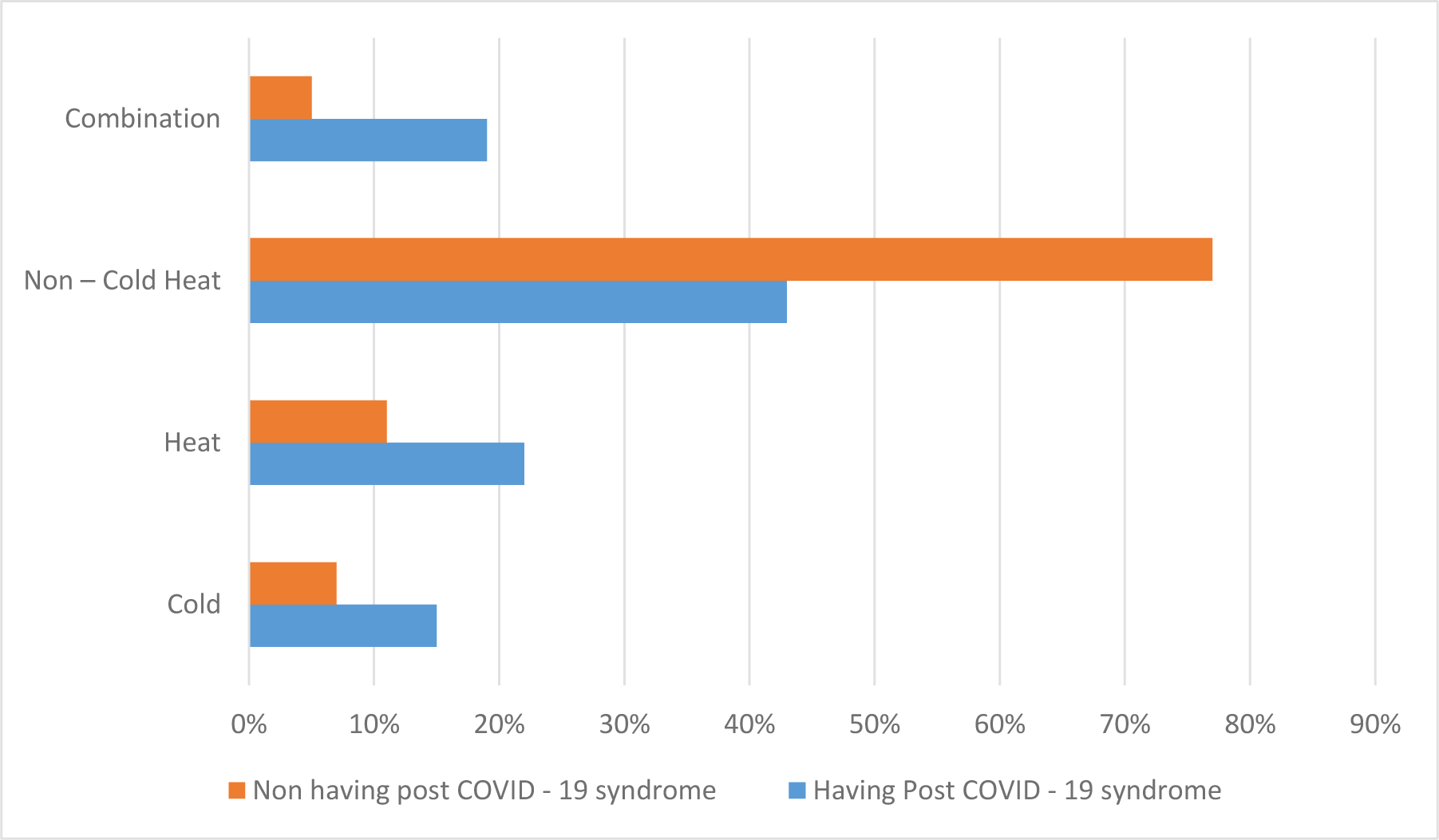
The Cold-heat patterns ratio in post-COVID-19 groups illustrated highly dissimilarity to the other group. Despite being the majority of both groups, the non-cold–heat in non-post-COVID-19 groups was 1.8 times as much as in the post-COVID-19 groups. On the other hand, the heat, the cold, and the combination in post-COVID-19 patients were higher than in people who did not. The contrasting ratio of the cold, the heat, and the combination between post-COVID-19 and non-post-COVID-19 respectively were 2.2 times, 2 times, and 3.8 times. P = 0.0003 (< 0.05), therefore, there was a relationship between the cold–heat patterns and the post-COVID-19 status.
4. DISCUSSION
The significant difference in gender where the female percentage was dominant, and the relevance between gender and post-COVID-19 status was similar to the conclusion of Bai F et al. (2022), Gebhard (2021), and Carod-Artal (2022). This study noted that women more often reported at least one persistent symptom than men, and considered females one of the post-COVID-19 syndrome risk factors, besides age > 50 and BMI >=23 [11-13]. There are currently no studies explaining the mechanism that causes women to experience more and longer post-COVID-19 syndrome than men. However, it is possible to rely on Rudroff T’s research as a clue to explore the mechanisms of the relevance between other post-COVID-19 symptoms and women. Rudroff.T, based on other authors’ studies, accounted for a significantly higher number and more persistent fatigue post-COVID-19 in women. The study mentioned three factors. [14] Firstly, Rudoff.T raised the role of psychophysiological factors. Gebhard et al. showed that after living or receiving treatment in social isolation due to COVID-19, women experienced more persistent psychological problems than men. They were also more susceptible to mental health problems. In addition, they bore more stress and burden in marriage and family than males. All these aspects increased the level of stress, depression, and anxiety in women [12]. Second place was the central factors (IL-6, inflammation, sex hormones). IL-6 levels (which were thought to be involved in prolonged inflammation - an important part of the pathogenesis of the post-COVID-19 syndrome) were higher in women infected by SARS-CoV-2 than in men [15, 16]. In addition, sex-specific differences in the regulation of hormonal stress and inflammatory responses might also contribute to the relevance of women with post-COVID-19 syndrome [17]. Observing women’s common diseases involving abnormalities of the immune system regulated by sex hormones, such as rheumatoid arthritis or systemic lupus erythematosus, strengthened the thesis [18]. When infected, women’s immune system’s response was more substantial, and virus clearance was more efficient than men’s [19]. Finally, pre-existing medical conditions or medical history were also involved in the existence of the post-COVID-19 syndrome. Both physiological and psychological influenced the appearance of symptoms of post-COVID-19 fatigue.
The current study found no relevance between BMI and Age with post-COVID-19 status. This result was not consistent with most of the studies performed, such as those by H.Crook (2021), L.Vimercati (2021), Arjun (2022), S.J. Halpin (2020), Rudroff T (2020), and Surde (2021). In other studies, the BMI group of inter-obese or pre-obese group or older age group (> 50 years) was associated with post-COVID-19 status [14, 20-23]. This difference can be explained through dissimilarity in sample characteristics and limitations in the sampling process.
In the sample, more than half of the participants (56.13%) had a BMI of Normal (18.5–22.49). BMI pre-obese or obese (>= 23) accounted for 33.05%, lower than most in other post-COVID-19 studies. In the study of Arjun et al. (2022), in the group with an average age of 39 (28.88 – 49.13), 36% of the participants had obese or pre-obese BMI [22]. In the S.J. Halpin study, the median age in the clinical group was 70.5 (20-93) and in the ICU group was 58.5 (34–84), and 59% of the participants had BMI in the obese, pre-obese group [23]. The median BMI of this study (21.97 (19.72–23.415)) was also lower than in other post-COVID-19 studies. Sudre et al. (2021)’s study noted that the median age was 42 (32 - 53), and the median BMI was 25.9 (23.0 – 30.3) [24]. L.Vimercati et al (2021)’s study showed that the median age was 45.4 (36.49 – 54.31), and the median BMI was 25.4 (22.63 - 28.4375) [21].
Subjects in this study had a median age in the middle-aged group (33 (24 – 42)), similar to the age group in previous post-COVID-19 studies, but the age was lower than mentioned. The dissimilarity may be explained by the inadequate sample size and the convenient, non-stratified sampling method, leading to an uncontrolled sample size that was sufficient to represent the population. Moreover, the online sampling method is a conspicuous barrier for those over 60 years old, making the average age group primarily middle-aged and young adults.
Thus, this can explain the difference in BMI >=23 and median BMI between this study and the studies mentioned above. Theoretically, with increasing age, the risk of weight gain rises, with weight usually growing in adulthood until about age 65. Therefore, the younger age of the sample may reduce the median BMI and the prevalence of obese or pre-obese BMI. In addition, the difference may come from objective reasons about the anthropometric characteristics of Vietnamese people, most of whom have BMI at a Normal level. The rate of obesity or pre-obesity (BMI >= 23) for Vietnamese people is lower than in other countries in the region and the world [25].
In the study sample, 68% of the participants had the post-COVID-19 syndrome, similar to the study of Ghosn et al (2021) with 68% of patients had post-COVID-19 syndrome [26]. Besides, according to the report of Carvalho-Schneider, 66% of patients had experienced this syndrome [27]. However, a systematic review illustrated that the prevalence of these syndromes was 43% (39% - 46%) [28]. This dissimilarity may come from the differences in sex, location, COVID-19 study community, and definition of time for the post-COVID-19 syndrome [28].
According to TCM, COVID-19 is an epidemic disease, the cause of which is dampness toxicity, categorized as an outsider. It spreads through the Wei Qi Ying Blood or the san jiao [29]. In the early stages, dampness toxicity may undergo cold or heat formation based on physical condition, climate, and environment. [29]. However, the most critical factor is the warm nature of the causative agent. Depending on the heat or cold formation and the spreading of the dampness toxicity, which corresponds to mild, moderate, severe, or critical forms in the acute stage [29-31]. The “Diagnosis and Treatment Guidelines for New Coronavirus Pneumonia (Trial Version 7)” of the National Health Commission of China [32] found the following common disease syndromes in the acute stage. (1) Mild cases included Cold–dampness obstructing the lung syndrome, and dampness–heat-accumulating the lung syndrome; (2) Moderate cases included Cold–dampness stagnating the lung syndrome, dampness–toxin blocking the lung syndrome; (3) Severe cases had Epidemic toxin blocking the lung syndrome and dual blazing of qi–Ying aspects syndrome. Finally, (4) Critical cases had Internal block and external collapse syndrome.
Qi and yin are the two most damaged components in the acute stage. Dampness toxic heat burns the fluid, causing loss of yin and, simultaneously, stagnating lung qi and injuring qi of the whole body [29-32]. Therefore, in the recovery stage, there are two common syndromes in patients after COVID-19: deficiency of lung–spleen qi syndrome and qi yin deficiency syndrome [32]. These two syndromes correspond to the appearance of symptoms having cold or heat nature, being consistent with the difference in the rate of cold-heat pattern in the current study.
Although the non-cold-heat pattern was dominant in both groups, the ratio of the non-cold-heat pattern in post-COVID-19 groups was smaller than in the non-post-COVID-19 group. On the other hand, the heat, the cold, and the combination pattern in people experiencing post-COVID-19 were higher than in people who did not. In addition, the study also showed a relevance between cold-heat patterns and post-COVID-19 status (p <0.05). This relationship might indicate that the yin and qi of the majority in the non-post-COVID-19 group were less damaged. In contrast, the group with post-COVID-19 syndrome showed that the qi and yin deficiency was more severe and manifested more clearly.
Although there are currently no studies on cold–heat patterns in people after COVID-19, studies show common syndromes in these subjects. The syndromes - having symptoms showing the characteristics of heat or cold in patients - can be considered similar to the change of cold and heat patterns, as mentioned in the study results. Tian F et al. studied 115 people discharged from the hospital: 29.6% had no symptoms (Non-cold–heat), 7% had the unresolved toxic syndrome (Heat), 26.1% had the deficiency of lung spleen qi syndrome (Cold), 19.1% had the deficiency of Qi Yin syndrome (Combination), and 18.3% had the deficiency of lung–spleen qi syndrome with the stagnation of dampness (Cold) [33].
However, the syndromes in Tian F’s study, which inclined to the cold pattern, were the majority. On the other hand, this study shows a relative distribution of the cold, the heat, and the combination in the post-COVID-19 group. This difference could be explained by sample differences in terms of age, BMI, or limitations on sampling. Besides, Tian F’s research focuses on hospitalized patients, which was different from the current study, including patients who have been treated in field hospitals and patients in the community.
This study had a small sample size and used a convenient sampling method. This study used the questionnaire to assess the reliability and agreement of Korean experts. Although the result was positive, we do need other pilot studies to evaluate the reliability and the agreement of the Vietnamese experts.
Moreover, online questionnaires make it difficult for patients over 60 years old to agree to participate in the study. Current data were cross-sectional data in a small group, so longitudinal studies are needed to determine the relations detected.
Conclusion
This study reconfirmed the relevance between gender and the post-COVID-19 status in other studies and identified a statistically significant relationship between the cold-heat pattern and the post-COVID-19 status. This result consolidated the alteration of the Cold-heat pattern according to TCM papers. By identifying the relationship between the cold-heat pattern and the post-COVID-19 status, this study took the initial step in understanding the Eight Principles, which can assist other research in indicating the general TCM characteristics of post-COVID-19 patients. Furthermore, a comprehensive outlook on TCM properties of post-COVID-19 syndromes can help the intervened research to be more effective, for instance, by selecting herbs with warm or cold properties or acupuncture methods based on the Eight Principles.