1. INTRODUCTION
Approaching a child with noisy breathing is a challenge for pediatric clinicians. Determining the nature of the abnormal breathing sound can aid in identifying the cause of that. For examples, stridor and wheezing both are generated from obstruction of airway but their pathologic origins are different. Stridor that is musical, high-pitched and may be heard over the upper airways or at a distance without a stethoscope is induced by extra-thoracic airway obstruction. Meanwhile, wheeze that is musical, high-pitched, heard during inspiration, expiration or both, is related to intra-thoracic airway occlusion. However, in some cases of upper-airway obstruction, tracheal sounds can become frankly musical, characterized as either a typical stridor or a localized, intense wheeze. Recognizing this “tracheal wheeze” is crucial clinically because when auscultated over the lung, it is often mistakenly taken for the wheeze of asthma [1].
Asthma, a cause of intra-pulmonary airway obstruction, presents with wheezing. On the other hand, congenital laryngomalacia accounts 70% of extra-thoracic airway obstruction cases in infants is characterized by stridor [2, 3]. Congenital laryngomalacia may exist up to 2 years of age but it is not common in children older than 1 year [3, 4]. Although asthma in children is usually associated with allergy, many young children develop non-atopic asthma as a consequence of recurrent episodes of virus-induced wheezing [5, 6]. In clinical practice, it is not easy to diagnose asthma in pediatric patients because of lack of evidence for the diagnostic criteria of this condition. As a result, some children that have persistent or recurrent wheezing are usually over-diagnosed with asthma.
Moreover, there is evidence for coexistence of gastro-esophageal reflux (GER) and laryngomalacia [7] as well as GER and asthma [8, 9]. Some asthma medications, including oral corticosteroids and beta-2 adrenergic agonists, were documented to increase esophageal acid contact times as well as reduce lower esophageal sphincter basal tone and contractile amplitudes in the smooth muscle esophageal body, respectively [10, 11]. Therefore, if laryngomalacia is misdiagnosed with asthma, treatment of asthma may enhance the GER and make the patient’s stridor worse as well.
2. CASE PRESENTATION
A 19 month-old-girl was admitted to our department with a diagnosis of uncontrolled asthma. Her mother said that she had had persistent “wheezing” since she was 2 weeks of age and it progressed. Her “wheezing” was worse during laugh and supine sleep. She also had choking if she was fed in the supine position. The child visited doctors at many medical centers and was diagnosed with asthma. She had used many asthma medications, including daily inhaled corticosteroids, but her symptoms have not improved yet. Her parents have really worried about her condition. At our request, her mother made a video-clip of her breathing during sleep. The clip illustrated that she had stridor, not wheeze, and increased working of breathing during her inspiration (S1).
Given that, congenital laryngomalacia is rarely seen in children older than 1 year. Therefore, many laboratory investigations were conducted to differentiate causes of her stridor, although congenital laryngomalacia was the most likely diagnosis of her persistent stridor. Examination of the ear, nose, throat and x-ray of the neck did not reveal any obstruction. A CT-scan of the chest with contrast also did not find structural abnormality of the respiratory system. The result of fiberoptic naso-endoscopy (FNE) illustrated features of laryngomalacia, including severe edema of the epiglottis and arytenoid cartilages, which collapsed into the vocal cords during inspiration (Fig. 1).
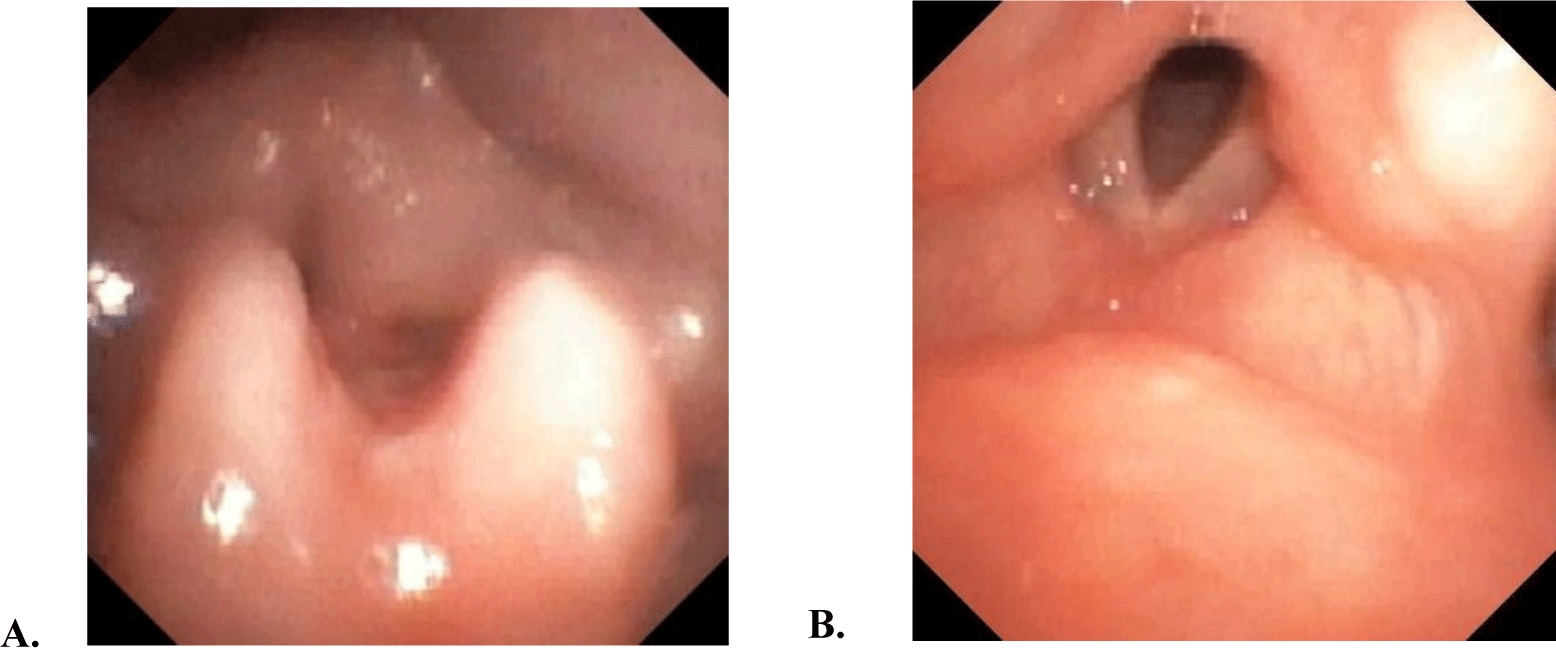
Additionally, because of the high coincidence of GER in infants with laryngomalacia, an upper gastrointestinal (UGI) endoscopy was also performed to rule out GER. No macroscopic appearance of GER was found, but histopathologic examination revealed microscopic features of chronic lymphocytic esophagitis, one of the complications of GER, in the tissue of the low end of the esophagus.
Following otolaryngology consultation, the patient was treated for GER for 1 month using Esomeprazole, solid feeding, and upright position during feeding, to minimize stridor with lateral recumbent position during sleep. We have planned to evaluate her stridor as the outcome of our management. If the stridor is not improved after 8 weeks of non-surgical therapy, we will perform FNE again to investigate further the obstruction and devise a better therapy. If her stridor is decreased, we are going to follow her up to 2 years old and will consider surgical treatment in need.
3. DISCUSSION
Stridor and wheezing are common symptoms of noisy breathing that bring children to clinics. However, in many cases, it is difficult to differentiate both of these breathing sounds [1]. As a result, some patients are misdiagnosed and incorrectly managed. Notably, observation of breathing sounds combined with increased work of breathing in respiratory phases can point to a diagnosis. Stridor or wheezing with difficult inspiration suggest an extra-thoracic airway obstruction. On the other hand, abnormal expiration is a sign of intrathoracic occlusion.
In some cases, a history of labored respiration that exacerbates during exercise or sleep can be confused with asthma, especially in children over 1 year old. Therefore, it is important to be careful in taking history and performing physical examination of a child with noisy breathing to make the best appropriate diagnosis and management.
Although congenital laryngomalacia is the most common cause of stridor in infants and not common in older children, it may exist up to 2 years of age in cases [3, 4]. Aside from conducting static imaging studies, dynamic imaging investigations should be performed to completely overview the airway obstruction in relation to respiratory phases.
In addition to a high coincidence of GER and laryngomalacia, prolonged use of a variety of asthma medications also may have increased the risk of GER in this patient. A esophago-gastro-duodenoscopy was performed to investigate the findings of GER. A normal endoscopic appearance of the esophagus does not exclude GER in suspected children [12]. Notably, the patient had severe edema of larynx cartilages, an indirect sign of GER in a child with chronic stridor [13]. Therefore, histopathologic examination should be carried out to further look for GER in these patients. The observed association of gastro-esophageal reflux and laryngomalacia in this case is presumably due to the more negative intrathoracic pressure, which is necessary to overcome inspiratory obstruction, giving rise to the reflux. Conversely, a significant reflux may also exhibit pathological changes similar to laryngomalacia, especially enlargement and swelling of the arytenoid cartilages [2, 3, 7]. A 7-day course of high-dose oral corticosteroid has been related to increased esophageal acid contact times [10]. In addition, inhaled albuterol has been showed reduction lower esophageal sphincter basal tone and contractile amplitudes of the esophageal body smooth muscle [11]. Therefore, it is important to consider that when laryngomalacia is misdiagnosed for asthma, inappropriate use of asthma medications such as bronchodilators and prednisone can worsen GER, leading to more severe stridor in these children. According to The North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN) and The European Society for Pediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN)’s recommendations [12], a trial of Proton-pump inhibitors for 4 weeks was chosen to treat her gastroesophageal reflux disease (GERD).









