1. INTRODUCTION
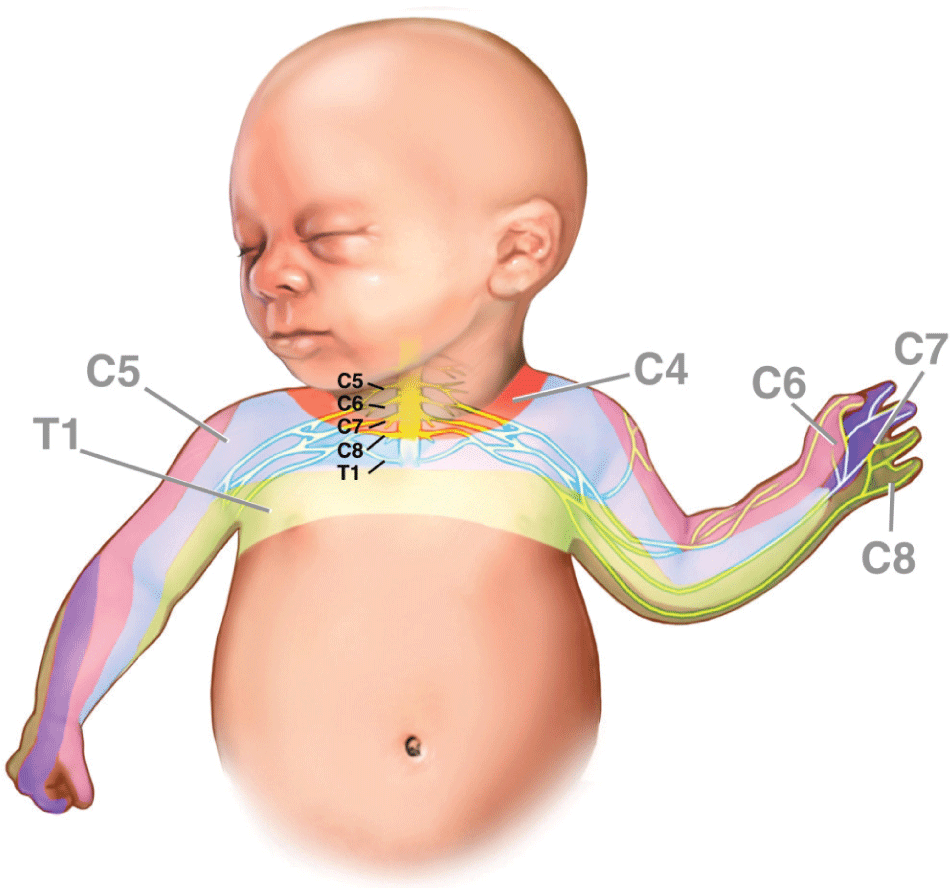
Post-delivery brachial plexus injury is an infrequent complication in newborn. Initial data on brachial plexus injury were described by Smellie in 1764 and Duchenne in 1872. As reported, brachial plexus injury incidence varied so much that it ranged from 0.15 to 3 per thousand live births by studies. This injury may spontaneously recover, data showed recovery rate ranged from 90 percent down to about 30 percent [1]. Brachial plexus is formed by nerve roots from cervical vertebra C5 to thoracic vertebra T1. Each root comes from the anterior and posterior spinal horns, integrates in spinal canal and goes out through intervertebral foremen (Figure 1). That is why the most accepted cause of brachial plexus injury is the over-stretch of fetal neck in the delivery phase of shoulder expulsion often seen in shoulder dystocia. This action will increase cervico-shoulder angle causing transient or permanent injury to brachial plexus in shoulder dystocia [1].
Tu Du Hospital is one of the leading hospitals specializing in obstetrics and new-borns with 2,000 patient beds. Tu Du is a central level hospital providing treatment, training and research services. The hospital is appointed by the Ministry of Health as the highest level of referral for 32 provinces/towns in the southern Vietnam. More than 65 thousand babies are born here each year. In clinical practice, we found many cases of brachial plexus palsy without shoulder dystocia.
Objective: To describe clinical characteristics and outcomes of 10 brachial-plexus injury cases among infants without history of shoulder dystocia.
2. CASE SERIES
Method: we conducted a retrospective analysis of ten cases with brachial plexus injury on monitoring and treatment at Tu Du Hospital Department of Functional Recover. We recruited those cases by using total sampling method. All ten cases without history of shoulder dystocia were selected among cases diagnosed brachial plexus injury that ICD-10 code were S14.3 from January to November 2018.
As per Mallet’s classification [1] based on brachial postures and functions (Table 1), there were seven cases with minor injury (Grade IV), three with moderate injury (Grade III) and none of serious injury (Grade II). All those cases were delivered in hospital including eight vaginal deliveries (five forceps deliveries) and two cesarean sections. There were two pre-term births with gestational ages of 35 weeks plus six days and 36 weeks, the remaining cases were full-term births. Female infants accounted for 6 and the remaining 4 were male. There was one transverse fetal presentation only among ten cases, and it was delivered through cesarean section, the rest was cephalic presentation. The cases with birthweight of 3500g or more accounted for 50 percent, a case had birthweight of 4500g but shoulder dystocia note was not recorded. Prolonged second stage of labor occurred in three cases. All the cases had unilateral injury and were treated with physiotherapy. Almost all infant patients were monitored at outpatient clinic and recovered within three to six months (Table 2).
All the injured arms or hands were recovered well without any sequela or limited movement.
3. DISCUSSION
On maternal end, the risk factors of brachial plexus injury include obesity, diabetes mellitus, history of large fetus delivery, shoulder dystocia and history delivery of brachial plexus injured newborn. In our ten cases, there was one case with pregnancy diabetes only, and no cases with history of large fetus delivery, shoulder dystocia [2]. As per Deaver JE et al., mothers with diabetes mellitus, high body mass index, high weight gain, together with black race and high fetal weight increased the risk of brachial plexus injury to 2.3 - 4.8-fold [3]. Nonetheless, some other studies showed maternal diabetes mellitus had no relation with newborn injuries in general (including brachial plexus injury), but body mass index of more than > 30 kg/m2 increased the traumatic risk. Regarding the maternal history of pregnancy, according to Hudic I, primi- or multi-parity did not make much difference [4]. However, the history of large fetus delivery or shoulder dystocia, history of brachial plexus injured newborn delivery had relation with brachial plexus injury in the following pregnancies [4].
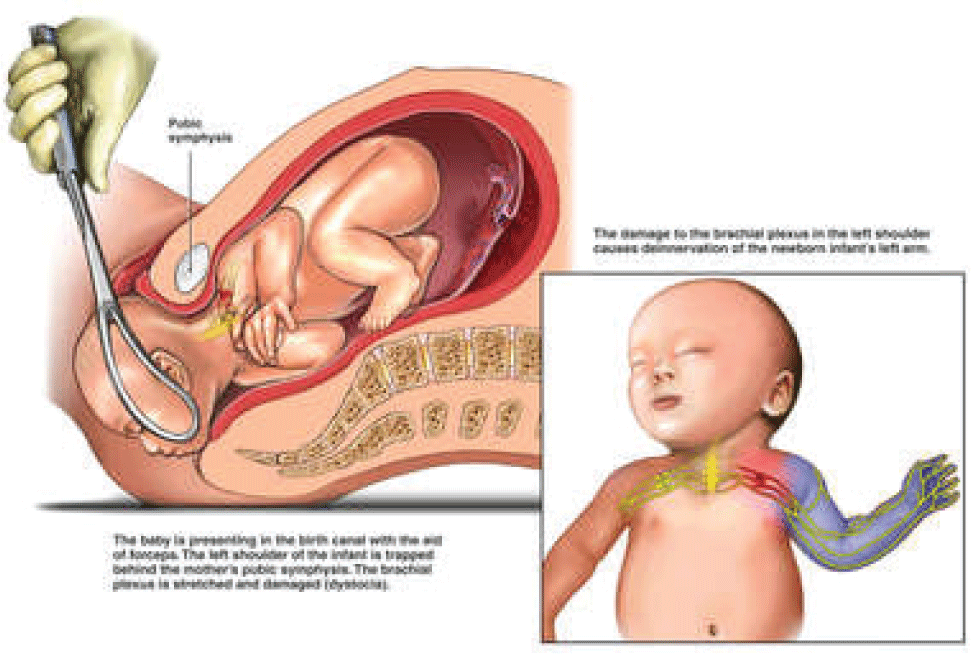
The risk factors during labor include breech delivery, prolonged second stage of labor, interventional delivery, shoulder dystocia. Okby et al. found breech delivery increased the risk of brachial plexus injury 36-fold. Many other authors also agreed with this remark [5]. Yet, Krause Met al. noted in a study in 2000 there was 1/796 (1.2/1000) of brachial plexus injury only in breech delivered newborns with gestational age of more than 32 weeks, which was not much different from the incidence of brachial plexus injury in newborns of cephalic delivery [6]. In our study there were no breech deliveries, three cases of prolonged second stage of labor. However, the correlation between the second stage duration and brachial plexus injury has not been clearly demonstrated and agreed. Interventional delivery was demonstrated as an independent risk of brachial plexus damage. There were 50 percent of cases in our study delivered with forceps. As per Foad SL’s notes, forceps delivery increased the risk of brachial plexus injury to nine-fold [7] (Figure 2). Cesarean section can partly protect, but it cannot fully exclude brachial plexus injury. In our report, there were two cases with cesarean section of which one case was transverse presentation in adenomyosis uterus and the surgical process was difficult in fetal extraction. The other case was emergency cesarean section due to fetal distress in non-obese and non-diabetic mother, cephalic presentation, with birthweight of 3400g. In 2016, Mohammad M. Al-Qattan reported a case with Klumpke’s palsy after emergency cesarean section for a newborn of 2800g and the maternal history of pregnancy was normal [8]. Some studies disclosed that cesarean section did not decrease more brachial plexus injury incidence than vaginal delivery. Shoulder dystocia is the most common risk factor of brachial plexus damage [7-9]. According to Foad SL et al., shoulder dystocia increased the risk of brachial plexus injury up to 100-fold [7]. Shoulder dystocia often occurs in newborn with heavy weight, but still in newborn with moderate birthweight. Other studies reported brachial plexus injury still happened in newborn without shoulder dystocia [9].
On the newborn end, together with shoulder dystocia, large fetus and clavicle fracture are also the frequent risk factors of brachial plexus injury. In our survey, no cases of clavicle fracture were noted, 50 percent of cases were large fetus (≥ 3500g). As per Foad SL et al., newborn with birthweight of more than 4500g had a 14-fold increased risk of brachial plexus injury [7]. However, some other studies reported brachial plexus injury still happened in cases with normal birthweight [7-9].
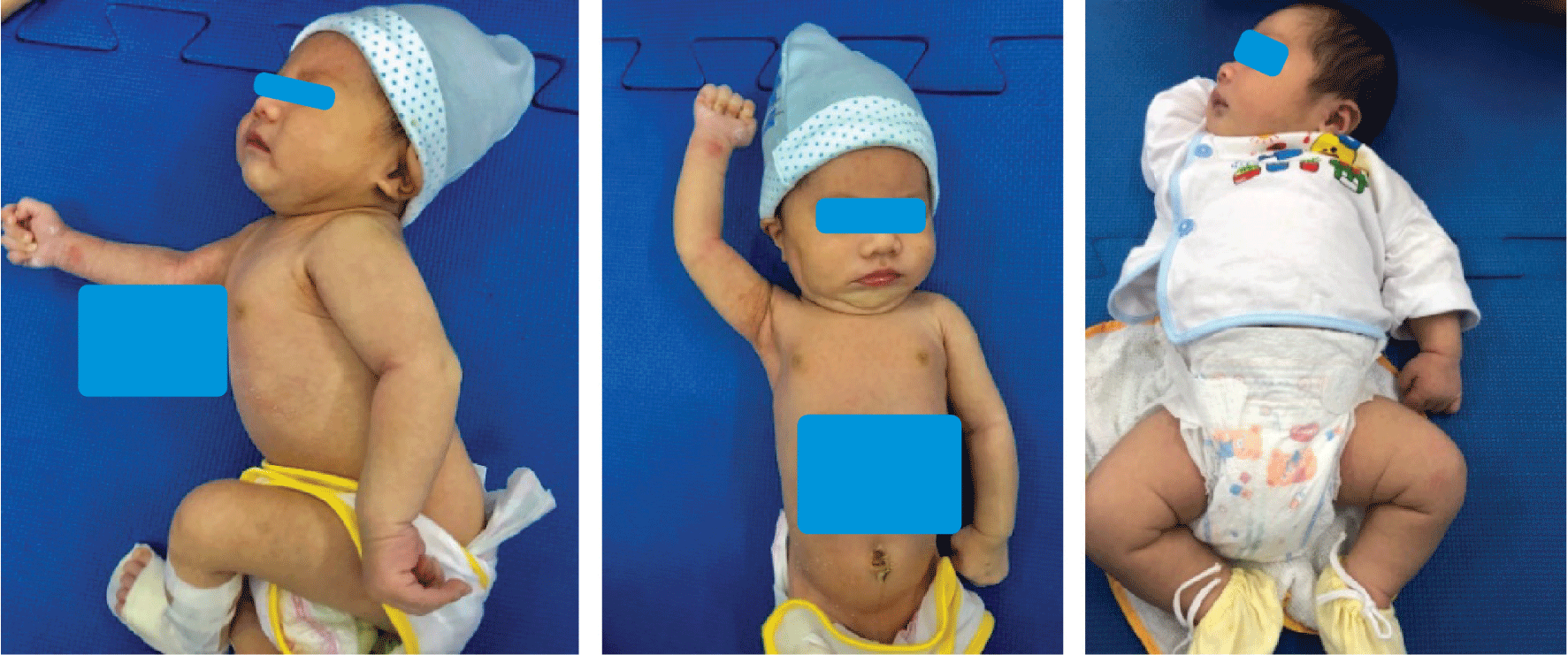
All our cases were detected early after birth mainly based on history of newborn dystocia, interventional delivery, birthweight, clinical symptoms like weak mobility at one arm or swelling at injured shoulder area and clinical examination (Figure 3). Coroneos et al. published his study on BMJ journal in 2017 with the following recommendations: first, examination to fi brachial plexus injury if the newborn had signs of mobility imbalance in two arms or such labor problems as shoulder dystocia, clavicle fracture, humeral fracture and so on; second, those infants need to be referred to relevant specialty institutions within one month after birth if brachial plexus injury is in question. Finally, there should be collaboration between internal medicine physician and neuro-surgery physician in the management of brachial plexus injury [9].
X-ray is the imaging method of choice, and can reveal clavicle or humeral fracture, or even shoulder dislocation. MRI and electromyograph are less frequently used, and for complex cases only. The main management is physiotherapy and follow-up at out-patient clinic. Vasileios Skoutelis in 2015 reported that hydrotherapy in combination with physiotherapy may well improve the infant’s motility capacity [10]. In our ten cases, all were well improved in motility after treatment. According to studies, recovery prognosis would depend on the extent of injury, time of injury detection and therapy approach. By some studies, the recovery rate after two years was 80% up to 96% and even, up to 98% after 18 months [6][7].
4. CONCLUSION
Brachial plexus injury is not a frequent complication in obstetrical practice, almost all cases are self-recovered. However, if serious injuries are ignored or late detected, recovery may be slow or long-term complications may remain due to untimely intervention. Brachial plexus injury could be happened even though infant delivered without history of shoulder dystocia. Therefore, in obstetrical practice, it should be early detected for maternal characteristics (such as diabetes mellitus, obesity), fetal characteristics (such as large fetus, clavicle fracture) and labor issues (such as abnormal presentations, prolonged labor, assisted delivery...) to set up appropriate management. As a result, newborn injuries in general and brachial plexus injury in particular will be limited.